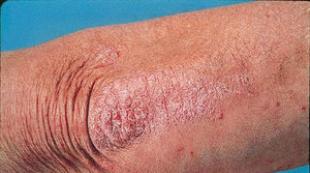
If your child has frequent fractures. Features of various types of fractures in children: associated symptoms, diagnosis and treatment, causes of frequent bone injuries
Last article updated: 05/02/2018
Every mother knows how active children are. The cognitive activity of children is very high. A child must constantly move, explore the world and learn new things. A broken leg or arm in a child is a common and very common occurrence. But, unfortunately, the child’s high energy, underdeveloped vestibular apparatus and imperfect sense of balance often lead to trauma. Often the little one falls, gets bruises, abrasions and even fractures.
Pediatrician, neonatologist

This depends on the age and psychophysical development of the child. Preschoolers are more likely to experience household injuries, falls, and burns. Among school-age children, street and even transport injuries predominate. Riding fast on bicycles, skateboards, roller skates, and failure to comply with traffic rules leads to serious consequences.
Features of childhood injuries
Children are not a smaller copy of an adult. The structure of a child’s body, as well as the musculoskeletal system, has a number of features. Many lesions typical of children are never seen in adults, and vice versa. Why is this happening?
High percentage of soft tissue

 In a growing body, the content of cartilage, fat and muscle tissue is greater than in adults. This feature has a protective function, so bones in children break much less frequently than in similar situations in adults.
In a growing body, the content of cartilage, fat and muscle tissue is greater than in adults. This feature has a protective function, so bones in children break much less frequently than in similar situations in adults.
High elasticity and firmness of fabrics
Due to the strength and elasticity of the periosteum, displaced fractures are rare. The periosteum, as it were, “holds” the fragments inside; such fractures are called the “green branch” or “rubber tube” type.
What is periosteum and why is it needed? The periosteum is a dense membrane that completely covers the bone. It is perfectly vascularized, supplied with blood, which means it nourishes the surface layers of the bone. Thanks to the periosteum, the bone grows in thickness.
High elasticity of ligaments
The ligamentous apparatus of children is highly elastic. Therefore, sprains and hyperextensions of ligaments are much more common than ruptures, and dislocations before 5 years of age practically do not occur.
The special mineral composition of bones
The bones of children are thin, but they contain a lot of organic matter. Bones have great elasticity and flexibility, which also protects against fractures.
How does bone growth occur? The growth zone is a cartilaginous layer. It is located between the articular part of the bone (epiphysis) and the expansion at the end of the bone (metaphysis) and allows the bone to grow in length.
Bone fractures in the growth plate
Such lesions occur only in children. But it is very difficult to identify them, because cartilage tissue is not visible on an x-ray. This is serious damage that requires proper, qualified treatment and precise comparison of surfaces.
Damage to cartilage tissue
 Cartilage tissue is not prone to fractures due to its homogeneous structure and elasticity. But with mechanical impact, the structure of the cartilage, its properties and content can change, and the cartilage can move and be reabsorbed.
Cartilage tissue is not prone to fractures due to its homogeneous structure and elasticity. But with mechanical impact, the structure of the cartilage, its properties and content can change, and the cartilage can move and be reabsorbed.
High reducing power
Over time, a callus forms in the affected area, which is replaced by bone tissue without scar formation. And the rapid growth rate of the child allows for a “permissible displacement” to remain, which can correct itself over time.
Types of injuries in children
The most common injuries in children include bruises, dislocations, sprains, and fractures.
- Injury. How to distinguish a bruise from a fracture and other injuries? In case of a bruise, the tissue damage is minor, and its structure is not changed. Pain is the main symptom of a bruise, but it is moderate, the baby quickly calms down.Limb shape and function are not significantly changed. There might be a bruise. The bruise formed by the impact evenly permeates the tissue. The child’s condition is not significantly affected; he soon forgets about the trouble.
- Sprain. This lesion is typical for children over 3 years of age, and the typical location is the ankle ligaments. Often the baby gets this injury when running, especially on steps, when the foot turns inward.The pain of a sprained ligament is acute, but the pain gradually subsides. Edema and swelling appear in the joint area. Movement in the foot is possible, but attempts to stand on the foot are accompanied by severe pain.
- Dislocation. It often occurs when a child falls and is characterized by disruption of the normal contours of the joints. When a dislocation occurs, the ability to move the joint is severely limited. The shape of the limb changes, it becomes deformed, shortened or lengthened. Local symptoms are quite pronounced: pain, swelling, hematomas.In children aged about 2 years, subluxation of the radius in the elbow joint, “pulling dislocation,” often occurs. It occurs when an adult holds a child’s hand tightly, and the child suddenly stumbles. With such an injury, the baby cries, spares his hand, holds it along his body.
- A child has a fracture. Fracture is damage to a bone, a violation of its integrity as a result of mechanical impact.
We will talk about this type of injury in more detail.
Main causes of fractures
- falls;
- domestic injuries;
- awkward movements;
- diseases leading to disruption of bone integrity;
- mutilation.
Depending on the type of fracture, its manifestations differ, but the main symptoms are similar.
Clinical manifestations of a fracture
- pain that intensifies with movement of the limb, palpation, touch;
- deformity of the affected limb;
- unnatural position of an arm or leg, attempts to bring the limb into a physiological position lead to severe pain;
- swelling at the fracture site, which increases very quickly;
- hematoma, bruise in the affected area.
Do not forget that any injury is a damage to the entire body as a system. The body responds to damage with both local reactions (pain, hyperemia, swelling) and general ones (weakness, malaise, fever). With severe multiple fractures and injuries to internal organs, even traumatic shock may develop.
Diagnostics
 How to distinguish a fracture from other types of injuries? To diagnose this type of injury, you need to know how the child was injured and under what circumstances. But parents were not always witnesses to an unpleasant situation. And a traumatized child, especially a younger one, will not be able to coherently tell the circumstances of the injuries.
How to distinguish a fracture from other types of injuries? To diagnose this type of injury, you need to know how the child was injured and under what circumstances. But parents were not always witnesses to an unpleasant situation. And a traumatized child, especially a younger one, will not be able to coherently tell the circumstances of the injuries.
It is necessary to determine the extent of damage, local reactions, abrasions, wounds, hematomas. And then pay attention to the position of the limb, whether the child can move his fingers.
Clinical manifestations of fractures can be divided into probable and reliable. Possible signs that help to suspect a fracture include swelling, hematoma, and dysfunction. Reliable ones that strongly indicate the presence of a fracture include the sensation of crunching of bone fragments and deformation of the limb.
You should always pay attention to the color of the skin around the injury, the mobility of the fingers and toes. A serious sign is paleness or cyanosis of the fingers combined with the absence of voluntary movements. This may indicate damage to a large vessel or nerve.
 Another serious symptom is the absence of a pulse and discomfort in the limbs, tingling, burning, or “pins and needles” sensation. In such cases, it is necessary to deliver the child to a medical facility as quickly as possible.
Another serious symptom is the absence of a pulse and discomfort in the limbs, tingling, burning, or “pins and needles” sensation. In such cases, it is necessary to deliver the child to a medical facility as quickly as possible.
Severe, open fractures (when the skin over the lesion is broken and a portion of the bone is visible) are rare in children. The danger of infection in such cases is great. Even less common are gunshot, infected fractures, which require serious, long-term treatment. More common are hand fractures of the “green twig” or “grapevine” type, which can be difficult to recognize.
An X-ray examination will help determine the exact type of damage. Only by confirming it X-ray can you be unequivocally confident in the correctness of the diagnosis. Rarely, in controversial cases, it is necessary to resort to magnetic resonance imaging.
What can be seen on an x-ray?
- the presence of a bone fracture;
- location of the fracture;
- is there a bias, is it significant;
- single fracture, or there are several fragments;
- what is the fracture line?
Main types of fractures in children
Child's leg fracture
- Femoral neck fracture. Sharp, unbearable pain in the hip joint, shortening of the affected limb. The leg is in an unnatural position - turned outward. And in the groin you can replace hematomas and swelling. Such symptoms indicate a displaced femoral neck fracture. If there is no displacement, the clinical picture is erased, the child can even walk.
- Patella fracture. It is characterized by pain in the knee, swelling, and possible bleeding into the knee joint. The function of the leg is impaired, attempts to bend the leg cause severe pain. When the fragments diverge by more than 5 mm, the supporting function suffers and the child cannot stand on his leg.
- Fracture of the leg bones. When both bones of the leg (fibula and tibia) are fractured, deformation of the limb, severe pain, swelling and pathological mobility of the limb are noticeable. If one bone is affected, the deformity is less pronounced, and active movements in the leg are preserved.It turns out that a fracture of the tibia, depending on the number of bone fragments and their location, can be classified as either mild or severe.
- Fracture of the foot bones. In addition to local manifestations of the fracture, support and motor function are impaired. Movements in the foot or attempts to stand on the leg lead to sharp pain.
- Heel bone fracture. The position of the limb is changed - the heel is turned outward. Swelling and pain appear, and the inability to move in the ankle joint.
- Fracture of toes. The fingers look unnatural, are swollen, and painful when moving. There is cyanosis and hematomas under the nails. The child cannot stand on his leg.
Child's arm fracture
Fractures of the upper extremities in children are 2 times more common than those of the lower extremities. With a serious fracture, it is easy to make an unmistakable diagnosis. But for children, lesions in which the function of the hand is slightly impaired are more common. A fracture can easily be mistaken for a bruise or dislocation. The most common location is in the bones of the elbow joint and forearm.
Urgent Care
Dr. Komarovsky shares advice on providing emergency care.
What to do:
- If there is bleeding, the first step is to stop it by applying a pressure bandage.
- Perform immobilization and fix the limb. Attach any flat object that is at hand with a bandage or cloth to the affected area.
- Apply cold.
- Immediately transport the child to the emergency room.
What not to do:
- Move the child until the limb is fixed and immobilized.
- Ask the victim to move, stand up, change seats.
- Try to change the position of the limb yourself - straighten it, align the fragments.
- Apply heat, rub, massage the damage.
Treatment of fractures
A qualified traumatologist will determine the type and amount of treatment required for each case individually. But there are basic principles for treating all fractures:
- Gentle approach, pain relief.
- Comparison of bone fragments is carried out in the shortest possible time, as quickly as possible.
- Surgical treatment if necessary.
- Fixation of the damaged limb.
- Conducting functional treatment.
Unconventional treatment and prayers for fractures are ineffective in treatment. By wasting time on traditional methods of treatment, you can miss precious minutes and harm the child. Only a qualified doctor can competently and correctly prescribe treatment.
Recovery period
How long a fracture takes to heal largely depends on the age and regenerative ability of the patient’s bone tissue. On average, the healing time for fractures of the upper limb is one to one and a half months, and for fractures of the lower limb - 1.5 - 2 months. Healing of a fractured pelvic bone will require even more - from 2 to 3 months, and for the spine the healing period will last up to 1 year, and complete recovery - 2 years.
 Healing time also depends on the type of fracture and treatment tactics. For example, with a simple fracture of the leg bones, a plaster splint may be applied for a period of 6 to 7 weeks. But in cases where it is impossible to combine the fragments with your hands, they resort to reposition using skeletal traction for a period of 4 - 8 weeks, followed by plaster casting. This means that the healing time of the shin bones doubles.
Healing time also depends on the type of fracture and treatment tactics. For example, with a simple fracture of the leg bones, a plaster splint may be applied for a period of 6 to 7 weeks. But in cases where it is impossible to combine the fragments with your hands, they resort to reposition using skeletal traction for a period of 4 - 8 weeks, followed by plaster casting. This means that the healing time of the shin bones doubles.
After removing the plaster cast, the active recovery period begins. The best methods of therapy at this time are massage, physical therapy, physiotherapy, and a swimming pool.
Do not forget about proper nutrition of the child and the increased need for microelements during the recovery period. Vitamin-mineral complexes, which include calcium, will increase regenerative processes and accelerate fracture healing.
In case of severe injuries, sanatorium treatment and long-term rehabilitation may be required.
Conclusions
All children are injured. This is a payment for the curiosity and activity of the baby. No matter how loving and caring parents are, they are not able to protect the baby from all possible troubles.
The main task of parents is to recognize the injury, be able to provide emergency assistance and, if necessary, transport it to a medical facility in a timely manner. The health and development of the child in the future depends on the correctness and speed of providing first aid and medical aid.
(No ratings yet)
She graduated from Lugansk State Medical University with a degree in Pediatrics in 2010, completed an internship in the specialty “Neonatology” in 2017, and in 2017 was awarded category 2 in the specialty “Neonatology”. I work at the Lugansk Republican Perinatal Center, previously in the neonatal department of the Rovenkovsky Maternity Hospital. I specialize in nursing premature babies.
Nowadays, young children and teenagers very often break the bones of their arms and legs. This school year, three students in our class, including me, broke their legs, and two more classmates were hospitalized with dislocations and partial fractures of their arms. I decided to find out why bone fractures occur and whether it can be prevented.
Selected research topic relevant, since in the last few decades in Russia 1 the incidence of limb fractures has been increasing, especially in children.
Purpose of the study: determination of the causes of fractures of limb bones and methods of preventing the occurrence of fractures.
study theoretical material about the structure of bones, types of bone fractures, prevention of childhood injuries;
conduct a survey of students;
learn to provide first aid for broken limbs;
prepare booklets for classmates on ways to prevent bone fractures.
Research methods: information analysis, questioning, observation.
Research hypothesis lies in the assumption that fractures of limb bones occur due to non-compliance with safety rules.
Object of study: bone fractures.
Subject of research: causes of bone fractures.
Chapter 1. Theoretical foundations for the study of bone fractures
Interesting facts about the human skeleton
Having studied the encyclopedia “Human Anatomy”, we found out that the word “skeleton” translated from ancient Greek means “dried up” - not a very suitable name for the engineering miracle created by nature that supports you and gives your body its shape. The skeleton consists of a large number of bones, they are connected to each other and form a strong and light supporting frame. The bones are alive. They are formed by bone tissue, a type of connective tissue supplied with nerves and blood vessels. But the skeleton is not just a support system. Muscles are attached to bones and allow us to stand, walk, run and jump.
The bones of the skull and ribs provide protection for fragile and delicate organs such as the brain and heart. The skeletal system of the hands, which accounts for a quarter of all bones in the body, allows you to write, sew, and perform other complex work.
We were very surprised to learn the fact that when a child is born, there are about 350 bones in his body, and the skeleton of an adult consists of 206 bones. So where do the 100+ bones go? The phenomenon of “disappearance” of bones from the body is explained by the fact that as a person grows and matures, the human skeleton undergoes numerous changes, and many bones, especially small ones, grow together to form larger formations. Skeletal growth stops at age 24.
So, we found out that in the adult human body there are more than 200 bones of different sizes. So, the shortest bones are the three bones inside the ear. Of these, the smallest is called the stapes (stirrup). Its length is slightly more than 3 mm.
The longest bone in the human body is the femur, which bears the weight of the entire body. It makes up ¼ of a person's total height. This bone has a saber shape and normally withstands the mechanical effects of blows, falls or compression, and can withstand pressure loads of up to 1500 kg. Damage to the hip bone is extremely dangerous and can lead to complete immobility in old age.
The most “bony” part of the body is the hands along with the wrists. It consists of 54 bones, thanks to which a person plays the piano, smartphone, and writes.
Human bone is both light and strong at the same time. It is 6 times stronger than a steel rod of the same weight! But if, nevertheless, our skeleton consisted of steel bones, then the weight of the skeleton would reach 240 kg!
Bone is an organ consisting of several tissues (bone, cartilage and connective) and has its own vessels and nerves. Each bone has a specific structure, shape, and position that are unique to it.
Bones are composed of organic and inorganic substances. Organic substances help bones to be elastic and elastic. Inorganic substances (phosphorus, magnesium, sodium, calcium) make bone strong. The chemical composition of bone is largely determined by a person's age.
A healthy person should have strong bones. However, there are some factors that affect their strength, as a result of which a person can break his arms, legs, spine, etc.
Types of fractures
Fractures are bone injuries in which their integrity is compromised. Fractures can be classified according to several criteria. Modern classifications distinguish the main types of fractures:
1. due to the occurrence:
traumatic - caused by external influences;
pathological - arising as a result of any disease;
complete without displacement and with displacement of fragments;
incomplete, i.e. cracks and breaks;
3. according to the integrity of the skin:
closed fractures, in which living tissue around the fracture site is not damaged;
open bone fractures accompanied by soft tissue injuries, as well as damage to human skin.
Fractures of the lower extremities include:
Fractures of the upper extremities include:
A fracture has signs that indicate that a fracture has occurred. This:
Pain- intensifies at the fracture site when pressed or loaded. For example, tapping the heel will sharply intensify the pain of a broken tibia.
Edema- occurs in the area of damage.
Hematoma- i.e. a large bruise caused by damage to the vessels that carry blood in our body.
Absolute signs of a fracture:
unnatural position of the limb;
pathological mobility - the limb is mobile in a place where there is no joint;
crepitus (a kind of crunching sound) - felt under the hand at the fracture site, sometimes heard in the ear;
bone fragments - may be visible in the wound.
Causes of bone fractures in children
Vladimir Merkulov, professor, doctor of medical sciences, head of the pediatric traumatology clinic named after N.N. Priorova in Moscow, says that the statistics of childhood injuries indicate that bone fractures in children most often occur with minor injuries and trivial circumstances at home, on the street, on the sports ground, for example, when falling from a great height, while running or walking etc. Fractures of arm bones in children are 2 times more common than leg bones. The most common sites for fractures are the elbow and forearm bones. Fortunately, severe multiple injuries in children are not common and account for 3% to 10% of all injuries to the musculoskeletal system. A child's bones are more elastic and less strong than those of adults, so the risk of fractures in children is higher than in adults.
In addition to fractures that occurred due to negligence, inattention, or self-indulgence, there are a number of other reasons why they occur. It turns out that bone strength may decrease and doctors call this condition osteopenia. This means that your bone mineral density is below normal. According to various studies, disorders of this kind are found in every third teenager from 11 to 17 years old. There are five main risk factors:
calcium deficiency, the main “building material” for bone tissue;
poor nutrition- in addition to calcium, bones need protein, phosphorus, iron, copper, zinc and manganese, vitamins, and all these beneficial substances are usually present in those foods that children like least;
physical inactivity(sedentary lifestyle) – to build bone mass, movement is necessary, which loads and trains the bones;
“hormonal storm” - during the period of growing up, a child may experience disturbances in the functioning of the body;
diseases gastrointestinal tract, respiratory tract, liver, kidneys, thyroid gland.
Loss of bone density develops gradually and is impossible to notice by eye, but here are 5 reasons why you can determine that there is not enough calcium in the body:
teeth began to deteriorate, that is, caries appeared;
“for some reason” hair splits, nails peel and break;
from time to time there are pains in the legs, especially in the legs;
it is difficult to sit with a straight back in class, she gets tired very quickly;
if you have an allergy, due to which you need to limit yourself in nutrition and not eat dairy products and fish.
Even if only one of these symptoms is present, you should definitely go to the hospital, get tested and find out whether you really do not have enough calcium.
A sufficient amount of vitamins and microelements in the diet helps strengthen bones. Calcium, magnesium, phosphorus, manganese, vitamin D, C, K and B vitamins are required for strong bones. There are a huge number of foods rich in these microelements and vitamins. These include: yogurt, cheese, salmon, spinach, soy, sardines, collard greens, grains (such as brown rice).
Great harm to bones comes from:
Conclusions for Chapter 1.
Bones are a unique building material. A healthy person should have strong bones. However, there are some factors that affect their strength, as a result of which a person can break his arms, legs, spine, etc. Fractures can be classified according to several criteria. The causes of fractures can be domestic injuries and serious problems in the functioning of the body. Proper nutrition and an active lifestyle contribute to strengthening bones.
Chapter 2. Practical part
2.1. Research into the causes of bone fractures
Having studied the theoretical material, we decided to check for what reasons bone fractures occurred in our classmates.
Purpose of the study: studying the causes of bone fractures
Research method: A written survey of students who have experienced a broken bone.
Data processing method
Appendix 1).
Bone fractures occur in children of all ages.
The reasons for the fractures were cited by schoolchildren as carelessness, inattention, falling from a bicycle, and skating on the roadway.
Students prefer a wide variety of foods, both healthy and unhealthy.
Most of the children, when asked if they play sports, answered yes, and they themselves write that in their free time they like to play with a tablet, computer, draw, and watch TV.
All the guys who were treated after a fracture noted that they were scared before the injections, they felt constant discomfort, and their mood was often sad and melancholy.
The students advised all the children to be careful, follow safety precautions, and not fall.
To find out food preferences, all students in the class were asked to fill out questionnaire No. 2.
Purpose of the study: Determining the effectiveness of the class students’ diet for strengthening bones.
Research method: written survey of class students.
Data processing method: data analysis and synthesis.
The survey results were summarized in visual diagrams ( appendix 2).
Analyzing the responses received, we made the following conclusions:
The consumption of fresh vegetables and fruits is not constant in the diet of children.
Onions, garlic, parsley, dill are consumed only some of them daily in small quantities.
Fermented milk products are not consumed daily by the vast majority of the class.
Most of all, children prefer baked goods made from premium flour.
Fish dishes are rarely consumed.
Most of all, students like to drink sweet carbonated drinks.
Schoolchildren most often eat mashed potatoes as a side dish.
Sweets are a favorite treat.
Most of all, students love “junk” (fried, fatty, smoked, pickled) food.
The survey results indicate that more than half of the students in the class are at risk. Such eating habits do not contribute to strengthening bones and maintaining the health of schoolchildren. The survey data give reason to assume that, in addition to negligence and failure to comply with safety regulations, bone fractures can also be caused by “weak” bones due to poor diet and sedentary lifestyle.
2.2. Prevention of childhood injuries
The problem of bone fractures is serious. What can be done to avoid them? I addressed this question to my grandmother Tatyana Pavlovna Krivenko, who works at the Tulun City Hospital in the dressing room for traumatology. She advised me and my classmates:
adhere to proper nutrition, avoid “bad” foods (chips, soda, sweets, soda), try to eat more foods containing calcium, phosphorus (fish, dairy, meat products);
spend more time in the sun to get vitamin D for your body;
lead an active lifestyle, move more, play sports;
do not have bad habits;
lift weights correctly;
correctly distribute time for work and rest, do not strain the body.
Follow safety rules when playing sports, playing games, or riding a bike.
2.3. Providing first aid for fractures
It is very important to be able to provide first aid to a person. As it turned out during an oral survey of classmates, no one knew how to do this. This was taught to us by Elena Vladimirovna Serebrennikova, Deputy Director for Life Safety and Information Environment of the educational organization.
Often, a severe injury can cause a bone fracture. In these cases, the first thing you need is complete rest for the damaged area of the body. To create immobility (immobilization) in the area of the fracture, the leg must be placed on a board, plywood or thick cardboard and bandaged to the leg. In case of fracture of the arm bones, immobilization can be achieved by placing the arm, bent at the elbow joint, on a wide scarf, the ends of which are tied around the neck or the damaged limb is bandaged to the body. Thanks to immobilization, pain decreases, the patient's condition improves, and he should be urgently taken to a doctor in the trauma department.
A rule that must be taken into account when immobilizing a damaged area:
it is necessary to fix the limb in the position in which it is after the injury and you should not try to set the bone in place, because this may cause even greater injury;
It is necessary to fix at least 2 joints (above and below the fracture). If there are wounds, you first need to treat the wounds, stop the bleeding, and only then apply splints.
Further treatment of fractures should occur under the supervision of doctors.
Conclusions for Chapter 2.
During the research work, a large amount of literature was read and a lot of information was studied on the Internet.
We have put forward a hypothesis that children can get broken bones only because of their carelessness and failure to comply with safety rules. Our hypothesis was partially confirmed. In addition to non-compliance with safety regulations, there are other certain factors that affect the degree of bone strength: diseases that a person has suffered, insufficient amounts of calcium and other minerals in the body, and a sedentary lifestyle.
While working on this topic, we realized that the causes of bone fractures can be both carelessness and the internal state of the human body. We cannot say whether the “culprit” for fractures in our class is a lack of calcium or other minerals, since none of the students have yet undergone an examination of the body to determine the amount of calcium.
The materials from our research were presented during class. We think that our classmates will have something to think about. Students were offered booklets containing information on the prevention of bone fractures. After all, everyone can minimize the risk of fractures. And the most important thing in life is health!
We plan to introduce the research materials to parents at the meeting. Perhaps this information will help parents adjust their children's diet.
In the future, I would like to continue studying the issues of promoting human health.
References
Andreeva T.M. Traumatism in the Russian Federation at the beginning of the new millennium / T.M. Andreeva, E.V. Ogryzko, I.A. Redko // Bulletin of Traumatology and Orthopedics named after N.N. Priorova. – 2007. – No. 2. – pp. 59-63
Richard Walker. Human anatomy. Illustrated atlas for children./ONYX 21st century. Moscow - 2001.
50 rules of healthy eating/Comp. G.S. Vydrevich. – M.: Eksmo; St. Petersburg: Tertsiya, 2007. – 64 p.
I explore the world: Children's encycl.: Medicine/Comp. N.Yu. Buyanova; Under general Ed. O.G. Hinn; Artist A.V. Kardashuk, T.V. Berezkina and others - M.: LLC "AST Publishing House", 1999. - 480 p.
Appendix 1
Results of questionnaire No. 1
7 students from the class who suffered bone fractures in different years of life took part in the survey.
Survey questions
When did you break your bones?
1 student - 2 times (at 3 years old and at 10 years old in the 2016 - 2017 academic year);
1 student - at the age of 4 he broke his leg falling from a bicycle;
1 student - broke his arm at age 7;
2 students - at the age of 10 in the 2016-2017 academic year - broke their legs;
2 students injured their hands at the age of 10 in the 2016-2017 academic year.
For what reason did you get a broken bone?
Skating in the wrong place – 2 (28.6%);
What is your favorite thing to eat?
Do you play sports?
What do you do in your free time?
What advice would you give to your classmates?
Observe safety precautions – 7 (100%)
Appendix 2
Results of answers to questions in questionnaire No. 2
18 4a grade students took part in the survey
source
The human body in the growth stage is able to accumulate calcium in its tissues. Thanks to this feature, a child's bones are much stronger than those of an adult, but this does not mean that children are less at risk of getting a fracture. Due to the increased physical activity characteristic of most children, their skeleton is constantly exposed to excessive loads. A small blow is enough for the bones to give way.
This often happens while a child is learning to walk. Lack of coordination and the ability to stand firmly on your feet makes it difficult to group the lower limbs when falling, which sooner or later leads to a predictable result - their damage.
Any injuries are classified, first of all, by their location. When talking about a broken leg in a child, we can mean damage to:
At the same time, one cannot ignore the specifics of the injury. Fractures are also classified according to the following criteria:
- maintaining the integrity of soft tissues;
- nature of damage;
- final position of the bone.
In medical parlance, a fracture is a violation of the integrity of bone fragments, but such an injury can also damage soft tissues. In this case, a laceration forms at the site of injury. Such fractures are called open. They have a number of characteristic differences from closed-type injuries, in which the integrity of the skin is not compromised:
Another important classification feature is the degree of bone tissue damage. Depending on the severity of the damage, fractures are divided into complete and incomplete (partial). The latter include:
With a partial fracture - fissure or subperiosteal - the structure of the bone as such is not disturbed. Thanks to this, its fragments remain motionless. Such injuries are called non-displaced fractures. They are difficult to diagnose, but they are more treatable.
The bone at the site of the chip is sharpened, which threatens soft tissue damage (open fracture). In addition, the displacement of fragments prevents the restoration of the entire structure. Without their return to the proper position, there is no talk of injury healing.
The younger the child, the more flexible his bones are. For this reason, fractures in preschool children are relatively rare and are almost never complete. Most children, after an unsuccessful fall on their leg, end up with a crack or subperiosteal “twig” without displacement of the chips.
Recovery from injuries in children is much more intense than in adults, due to the accelerated process of tissue regeneration. Of course, this does not mean that a child with a fracture does not need urgent medical attention. Moreover, the younger the child, the more dangerous it is to delay treatment of a damaged leg.
Without medical intervention, a broken bone may not heal properly. At the stage of active development of the body, this threatens irreparable deformation of skeletal fragments (for example, in the hip area) and disruption of musculoskeletal function. This is why it is so important to diagnose the problem in time.
To detect bone damage, it is not necessary to take your baby for an x-ray (although this procedure has been and remains the best method for diagnosing injuries). The fact that a child has suffered a fracture can be judged by its characteristic symptoms. Depending on the location of the damage, the clinical picture of the traumatic condition may vary.
Hip fractures present in different ways in children. The symptoms of injury directly depend on which bone was damaged. In addition, the clinical picture of a fracture of the neck and any other part of the femur with and without displacement varies greatly. Comparative characteristics of such injuries are presented in the table:
| Localization | Fracture without displacement | Displaced fracture |
| Upper part of the femur (greater or lesser trochanter) | Mild pain when walking, swelling | Impaired limb function (severe pain when moving) |
| Femoral neck | The pain is mild; when placing weight on the injured leg, the foot involuntarily turns outward | Severe pain that makes it impossible to lift the limb in a straight position, swelling of the groin, visual shortening of the limb |
| Mid thigh | Muscle swelling, hematomas, visual shortening of the femur | The same plus abnormal mobility of the femur, accompanied by a characteristic crunch, unbearable pain (up to the development of shock) |
| Lower thigh | Severe pain, dysfunction of the limb, accumulation of blood in the knee joint | The same, plus visible deformation of the upper part of the knee |
The following symptoms indicate that the ankle bone is damaged:
- pain in the ankle area;
- swelling of local soft tissues;
- extensive hematomas and hemorrhages;
- dysfunction of the joint (limited mobility of the foot).
In the human body, the lower leg is represented by two bones - the tibia and fibula. Both of them are thick and massive, it is difficult to damage them. For this reason, a tibia fracture is considered a specific injury, the symptomatic picture of which will directly depend on the source and nature of the damage received. Nevertheless, all such injuries have common signs:
A broken toe is the most difficult to identify. Conventionally, the symptoms that help to do this are divided into 2 groups:
- Probable. These include pain, redness and swelling of the soft tissues, an unnatural position of the finger and difficulties that arise when trying to move it.
- Reliable. 100% signs of a finger fracture are pronounced bone defects identified by palpation - pathological mobility, deformation, shortening, etc.
If any fall or blow results in injury for the baby, he probably has a pathological predisposition to fractures. This is the name for a condition in which the integrity of the bone structure is disrupted due to internal changes occurring in the body. Pathological fractures are often caused by the following diseases:
- osteoporosis;
- osteomyelitis;
- new bone formations.
The main reason for violating the integrity of bone tissue is a strong mechanical impact - impact. However, the same fall can cause different injuries in children. One child will get away with a bruise, and the other will spend a good amount of time healing a fracture. The main risk factors that contribute to a decrease in bone strength include:
- Calcium deficiency. This substance is the main building material for bone. Therefore, children need to consume more foods containing calcium (milk, kefir, cottage cheese, meat, etc.).
- Sedentary lifestyle. To keep bones strong, a child must be physically active.
- Hormonal disorders. In this regard, the largest number of fractures is observed in children who have entered puberty.
Some chronic diseases can also interfere with the normal absorption of calcium. It is necessary to consult a pediatrician if your child’s hair begins to grow dull and fall out, caries develops rapidly, and the back gets tired quickly.
Injuries in children differ from those in adults. For a child, a “green stick” bone injury is typical, in which the fragments are held in place by strong periosteum that has preserved its integrity.
Damage to the joints in children is fraught with damage to the cartilage of the growth zone, and therefore the lengthening of the limb after injury may stop. In general, healing occurs faster in a child than in an adult.
This process is accompanied by the migration of cells into the pathological focus, forming a section of new bone tissue (callus) at the site of a post-traumatic hematoma. In addition, when localized in the area of the cartilaginous growth zone, necrosis of the bone tissue of the epiphysis develops in children (traumatic epiphysiolysis).
Skull fractures are most often the result of a fall from a height or a traffic accident. Both the arch and the base may be involved in the pathological process.
The clinical picture of a fracture is characterized by the following signs:
- pain at the site of injury;
- swelling of the damaged segment;
- formation of a hematoma at the site of application of mechanical force;
Hematoma is a typical sign of a fracture in children
A skull fracture is characterized by the following symptoms:
- excruciating headache;
- episodes of loss of consciousness, convulsions;
- nausea and vomiting;
- leakage of clear cerebrospinal fluid (CSF) from the nose and ears;
- different pupil sizes (anisocoria) indicate accumulation of blood inside the cranial cavity;
Anisocoria is a sign of intracranial hematoma formation
Fractures in a child are usually very different from fractures in young and old people. If the baby falls or hits himself, the following types of fractures are most often observed:
- Subperiosteal fracture;
- Epiphysiolysis;
- Osteoepiphysiolysis;
- Apophysiolysis;
- Fracture of the periosteum.
Depending on the structure and strength of the patient’s bone, the following forms of fractures are distinguished:
- Traumatic. Damage develops due to strong mechanical impact on the bone (fall, blow).
- Pathological. Such fractures can develop even with mild physical impact and are a consequence of a certain disease.
Based on the condition of the epidermis, fractures in children can be:
- closed (the integrity of the epidermis is not compromised);
- open (elements of the damaged bone violate the integrity of the skin).
Closed fractures are not infected. Open fractures have primary microbial contamination. Therefore, first aid for different types of injury differs significantly.
Depending on the type of separation of individual bone elements, fractures with and without displacement are distinguished. For young and middle-aged children, subperiosteal fractures of the “green stick” type are most common. The peculiarity is that the damaged area does not lose the integrity of the periosteum. In most cases there is no displacement. This injury often develops in the lower leg or forearm.
Depending on the direction of the fracture line, the following types of injury are distinguished:
- star-shaped;
- transverse;
- longitudinal;
- oblique;
- helical;
- V-shaped;
- T-shaped.
According to the nature of the injury in children, fractures of the vertebral bodies are distinguished (compression, crushed, splintered), isolated fractures of the arches; transverse, spinous and articular processes of the vertebrae.
The most common injuries in young patients are injuries to the arms and legs. At the same time, about 5% are injuries to the hands and fingers. Most often, such injuries occur in children who are just beginning to take their first steps. Damage to the upper limbs can be caused by a bad fall.
Injuries in children of the first year of life are quite rare. If a child who does not yet walk or even sit is often diagnosed with fractures, it is possible that he had to deal with congenital osteoporosis.
Some babies may be diagnosed with birth injuries. Most often you have to deal with a fractured collarbone in a newborn due to the mother’s narrow pelvis. Malpresentation of the fetus is also a risk factor. Therefore, monitoring the woman and the condition of the baby in the last stages of pregnancy plays a very important role.
Children have a special bone structure. In this regard, in a child who is fully developing and does not have chronic diseases, the likelihood of getting a fracture is minimized.
Even if a young patient is diagnosed with an injury, the rehabilitation period is much faster than for an adult. Often in children of the first years of life, fractures of the bone outgrowths to which the muscles are attached are detected.
These are tears of ligaments and muscles with bone elements.
Treatment of fractures in children is complex and is carried out under the guidance of a pediatric traumatologist with the possible involvement of a neurologist and neurosurgeon. Uncomplicated cases are subject to treatment on an outpatient basis; if complications develop, hospitalization in a specialized hospital department is required.
If a child is injured, it is necessary to quickly and competently provide him with first aid. The following procedure must be followed:
- stop the action of the pathogenic factor;
- create immobilization of the fracture site using a scarf or scarf;
- in case of lack of consciousness, convulsions, vomiting, turn your head to the side;
- in case of an open fracture, apply an aseptic bandage to the damaged area;
- If your hand is injured, remove rings and other jewelry;
- In case of an open fracture accompanied by bleeding, apply a pressure bandage.

The effectiveness of first aid depends on strict adherence to the algorithm of actions
Children rarely have bone fractures, despite frequent falls during outdoor games; however, in addition to the usual fractures observed in adults, some types of fractures appear that are characteristic only of childhood, which is explained by the peculiarities of the anatomical structure of the skeletal system and its physiological properties in children.
Such fractures are a consequence of obstetric care for foot or pelvic presentation of the fetus. Typical localization is in the middle third of the diaphysis of the tubular bone; along the plane, the fracture runs in a transverse or oblique direction.
Traumatic epiphysiolysis of the proximal and distal ends of the humerus and femur are rare. This circumstance, as well as the fact that X-ray diagnostics are difficult due to the absence of ossification nuclei, often lead to untimely diagnosis of these injuries.
In diaphyseal fractures of the humerus and femur with complete displacement of bone fragments, pathological mobility at the level of the fracture, deformation, traumatic swelling and crepitus are noted. Any manipulation causes pain to the child.
Fractures of the femur are characterized by a number of features: the leg is in the typical position of flexion in the knee and hip joints for a newborn and is brought to the abdomen due to physiological hypertension of the flexor muscles.
There are several treatment options for newborns with diaphyseal fractures of the humerus and femur.
In case of a fracture of the humerus, the limb is immobilized for a period of 10-14 days. The arm is fixed with a plaster splint from the edge of the healthy scapula to the hand in the average physiological position or with a cardboard U-shaped splint in the position of shoulder abduction to 90°.
It is not difficult to suspect a fracture in a child. Immediately after the injury, the baby feels sharp pain and cries. The site of injury rapidly swells and acquires a bluish tint. A characteristic sign of a limb fracture is its deformation. In addition, the child may become pale, sticky sweat appears, and body temperature rises to low-grade levels.
Nonspecific symptoms may occur with greenstick fractures. The child can maintain physical activity and there will be virtually no pain. Often, it is possible to determine the presence of a fracture only with the help of hardware diagnostics in a hospital.
To establish a correct diagnosis, the following methods are used:
- thorough questioning to determine the circumstances of the injury;
- an objective examination of the damaged body segment allows you to identify hematoma, swelling, pain, and disruption of habitual movements;
When examining the damaged area, pain, swelling and limited mobility in the joints are revealed.
X-ray is the gold standard for diagnosing fractures in children

Computed tomography is a method for diagnosing skull fractures and traumatic brain injury
Differential diagnosis is carried out with the following diseases:
- tuberculosis of bones and joints;
- hematogenous osteomyelitis;
- arthritis of an allergic nature;
- arthritis of an infectious nature;
- juvenile rheumatoid arthritis;
Juvenile rheumatoid arthritis is characterized by severe joint swelling
If a fracture is detected in a child, it is strictly forbidden to self-medicate. Therapy should only be prescribed by a qualified specialist. At the same time, parents should know how to provide assistance to the victim before the ambulance arrives. The algorithm of actions should be as follows:
- Immobilize the damaged area using a splint. Any hard means at hand will do - a ruler, a board, a stick. As a last resort, you can roll up a magazine. If the tire turns out to be quite rough, wrap it in a bandage or towel before applying it. If a rib is fractured, a pressure bandage is applied.
- It is necessary to ensure that the splint is applied above and below the fracture joints.
- The splint should be carefully secured using a bandage. The bandage should not be too tight.
- To relieve pain, the child can be given a drug based on ibuprofen or paracetamol.
In case of an open fracture, before immobilizing the damaged area, it is necessary to treat it with an antiseptic and stop the bleeding. It is advisable to carefully remove clothing from the area of injury (it is better to cut it off).
In case of an open fracture, the doctor must clarify whether the patient has previously been vaccinated against tetanus.
For simple fractures without displacement, the prognosis of therapy is usually favorable. Children's bones heal quickly and their function is restored. The rehabilitation period in most cases does not exceed 3 months.
Displaced bone injuries require longer rehabilitation. It is often necessary to perform multiple surgeries to restore normal functionality to the injured area. The following complications are possible:
- injuries to nerves, ligaments and tendons;
- addition of a bacterial infection;
- improper fusion of bone, which leads to disruption of its functionality.
In most cases, if qualified assistance is provided in a timely manner, the child’s health condition is completely restored. However, unpleasant consequences of fractures are also possible. The most common complication is premature closure of the growth plate, resulting in deformed bone.
It is not always possible to protect a child from falls and injuries. But you can significantly reduce the likelihood of fractures if you monitor your baby’s diet. Food should be healthy and varied.
Physical activity is also of great importance. The child should regularly spend time in the fresh air and experience moderate physical activity.
The prognosis for treatment of fractures in children largely depends on the nature of the injury. Multiple injuries, crushed bones with complete loss of some areas complicate the situation. In severe cases, the following complications may develop:
- systemic reaction of the body to damage - traumatic shock;
- the body's systemic reaction to blood loss is hemorrhagic shock;
- wound suppuration;
- post-traumatic purulent inflammation of the bone - osteomyelitis;
- non-union of the fracture with the formation of pathological mobility of the bone area (false joint);
- formation of joint stiffness;
- limb deformity;
- shortening of the limb with the formation of lameness;
- lethal outcome.
It is necessary to explain to children the rules of safe behavior on the street, at home in child care institutions, and in transport. Young children require supervision.
There should be no dangerous objects that could cause injury in the room where the child is located. Small children must be transported in a car using a special restraint device.
Parents should feed their baby foods rich in calcium and phosphorus, as well as foods high in vitamins and minerals.
source
Of course, any person in his life is subject to such unpleasant phenomena as blows, bruises, dislocations, and fractures. The causes of these injuries are in most cases unsuccessful falls.
Childhood injuries are one of the first places in terms of frequency of cases, so in this article we will talk about what common causes of fractures in children are found, how to correctly assess the severity of the injury and how quickly the function of the damaged bone will be restored.
Medical statistics in traumatology practice show that fractures in children usually occur under everyday circumstances - fell at home, fell from a height, slipped on the street, jumped from a great height, landed unsuccessfully when falling from a bicycle, roller skates, etc.
The most common location of fractures in children is the bones of the forearm and elbow joint, followed by the bones of the lower extremities, in particular the toes. Unlike adult trauma, fractures in children in most cases occur without complications, which is due to the anatomical structure of the musculoskeletal system and the good ability of bone tissue to produce new osteocytes and heal.
The bones of a child contain a large amount of organic substances, in particular the protein ossein, which allows tissues to regenerate and grow together faster, unlike the bones of an adult.
The shell covering the bone from the outside - the periosteum (periosteum) is very elastic and dense, penetrated by a large number of blood vessels, and the bone itself has growth zones - metaphyses, which have plates of cartilaginous tissue. All these nuances of the structure of a child’s tubular bones make it possible to determine the specifics of fractures.
Table. Features of childhood fractures:
| Feature of the injury | What is it characterized by? |
| According to the “green line” type | Due to the high elasticity of the periosteum, when a child is injured, the bone does not break in half, but only cracks, which looks like a broken branch of a young tree. This type of injury is characterized by a bone fracture on only one side, and on the other side the fragments are firmly held by the periosteum. As a rule, displacement of bone fragments with this type of fracture practically does not occur or they are insignificant and not dangerous |
| Bone fracture line along the growth zone | A bone fracture along the metaphysis often leads to premature ossification of cartilage tissue, which causes subsequent shortening, curvature and impaired growth of the limb. In this case, the younger the child is at the time of receiving such a fracture, the more severe the consequences will be for him and the more pronounced the shortening of the limb will be. |
| Bone outgrowth fracture | Muscles and tendons are attached to the site of the bone growth, so when such a fracture occurs, ligaments and muscle tissue are torn |
Important! The periosteum in children is supplied with blood much better than in an adult, therefore, in childhood, callus forms more quickly and the fracture site heals.
Fractures in children can be pathological or traumatic, with the latter being the most common. Pathological fractures occur with the progression of various diseases, under the influence of which bone tissue is destroyed or there is a severe deficiency of vitamin D in the body - in this case, even the slightest knock or minor bruise is enough to damage the bone.
Traumatic fractures develop under the influence of a strong mechanical impact on the bone, short-term but significant.
In addition, fractures in children can be:
- open– the injury is accompanied by rupture of soft tissues, protrusion of the bone outward and quite severe bleeding, often threatening the life of the victim;
- closed– the integrity of the skin is not broken, and the bone fragments are isolated from the outside world.
Closed fractures are uninfected, while open injuries are necessarily a high risk of developing serious complications due to infection entering the wound.
Depending on whether there was displacement of bone fragments, fractures are diagnosed:
- with displacement - they are distinguished between complete displacement, when the fragment is completely detached from the bone and goes to the side, and with incomplete - fragments are present, but they are securely fixed by the periosteum and are not separated from the injured bone;
- without displacement - the bone is broken and held by the periosteum or the fracture is complete, but also a section of the bone is held by the periosteum.
Depending on the line of bone fracture:
Depending on the type and structure of the bones, they are distinguished:
- fractures of flat bones - these include the bones of the skull, ilium, and scapula;
- fractures of tubular bones are the most common types of injuries;
- fractures of spongy bones - calcaneus, vertebrae, talus.
Important! When spongy bones are fractured, they become compressed and their height decreases—this type of fracture is also called a compression fracture.
Tubular bone consists of epiphyses - the heads of the bone, diaphysis - the body and metaphyses - cartilaginous inserts, the so-called growth lines, located next to the epiphyses.
Depending on the location of the fracture of the tubular bone, there are:
- diaphyseal fractures;
- epiphyseal;
- metaphyseal.
The clinical picture of fractures in children varies depending on the location of the injury.
There are general signs characteristic of a fracture or fracture of a bone:
- Sharp pain – even if the fracture is not visually immediately noticeable, this injury in a child is accompanied by severe pain. The victim cries, is restless, and takes a forced position.
- Limitation of mobility - since any attempts to move the injured limb cause pain to the child, he tries to limit them, which is clearly visible from the outside.
- Swelling - swelling usually occurs at the site of bone damage, sometimes accompanied by a hematoma, which is caused by blood leaking from the bone cavity under the skin.
Important! Open fractures are easy to diagnose because the broken bone usually sticks out. This type of injury requires proper and immediate first aid, as it often causes massive blood loss and painful shock in the child.
The incidence of fractures of the pelvic bones is much lower than that of the tubular bones of the extremities, but this type of injury is much more severe and has a greater risk of complications. A fracture of the pelvic bones is accompanied by severe pain, severe pallor of the patient’s skin, and the inability to stand on his feet. Sometimes, from painful shock, the victim loses consciousness even before the ambulance arrives and attempts to provide him with emergency assistance.
A special group of fractures in children includes compression fractures of the spinal column, in particular of individual vertebrae. The main cause of this type of injury is a fall from a height onto the back. The insidiousness of a compression fracture of the spine is that the injury is difficult to diagnose, and all pain goes away on its own after 4-5 days.
Therefore, if you did not show your child to a traumatologist immediately after receiving a back injury, then with a high degree of probability the fracture will never be diagnosed, which is fraught with the development of many unpleasant conditions in the future, ranging from severe back pain to disorders of the nervous system due to compression of the spinal cord roots.
As mentioned above, the causes of frequent bone fractures in children of preschool and school age are, as a rule, household injuries caused by blows, unsuccessful falls, and landings from a height.
Predisposing factors to high bone trauma and bone fragility are the following conditions:
- lack of dairy products or fish in the child’s diet - often children categorically refuse milk, cottage cheese, kefir, fish, which leads to insufficient intake of calcium and phosphorus into the body - microelements necessary for strengthening bones;
- long-term therapy with hormonal drugs – prolonged use of hormones makes bone tissue fragile and the bone vulnerable to injury and damage;
- not frequent walks in the fresh air - in particular under open sunlight, since it is ultraviolet exposure to the skin that contributes to the production of a sufficient amount of vitamin D, which takes part in the formation of bone tissue cells and ensures the elasticity and strength of bones.
The causes of frequent fractures in adolescents are associated with increased intensive growth of the skeleton, as a result of which the bones do not have time to adapt to the changes that are occurring and cannot withstand the increased load. Plus, teenagers often actively engage in sports and at the same time eat irregularly and unbalancedly - all these factors together lead to fragility or insufficient strength of bones and the musculoskeletal system as a whole.
If you suspect a fracture in a child, then it is necessary to take the victim to the hospital - the doctor will assess the severity of the injury and prescribe adequate treatment with minimal consequences for musculoskeletal function in the future.
The main aspect of providing assistance to a victim with a fractured limb is to ensure its immobility so that the bone fragments do not move and injure healthy areas of tissue.
Below are instructions for providing first aid to patients with a closed fracture:
- Give the victim an anesthetic - since a fracture is accompanied by severe pain, before proceeding with fixation of the limb, it is necessary to reduce the pain threshold in order to avoid the development of pain shock. For a child, preparations based on Nimesulil or Ibuprofen are ideal - Nurofen, Nimesil, Nemidar and others.
- Securely fix the injured limb - this prevents bone displacement and injury from soft tissue fragments. If you don’t have any special devices at hand, you can fix the broken bone with two flat boards, wide rulers or plywood, tightly bandaging it. Important! Not only the broken bone should be fixed and immobilized, but also the adjacent joints, for example, in the case of a forearm fracture, the wrist and elbow.
- Take the victim to the hospital.
A fracture with a violation of the integrity of soft tissues requires special attention and caution in actions, since protrusion of the broken bone outward is accompanied by bleeding and a high risk of further complications.
If the wound is large and the bleeding is massive, you should quickly navigate and determine its type - venous or arterial, on which further actions will depend. With venous bleeding, the blood, which is a dark, rich red color, usually flows calmly. With arterial blood, the blood is scarlet, bright, gushes out and quickly leads to life-threatening complications.
Important! In case of an open fracture in a child with bleeding, first of all, you should give an anesthetic and only then quickly proceed to other manipulations.
To stop venous bleeding, a tourniquet or tight bandage is applied to the victim below the fracture site, always including a note indicating what time and by whom these actions were carried out. In case of arterial bleeding, a bandage is applied above the fracture site with the same note, after which they begin to treat the wound surface and fix the limb.
Important! If there is no bandaging material or rope suitable for the role of a tourniquet at hand, then you can tear the clothes into strips or firmly press the place of the torn vessel with your fingers and wait for an ambulance - all actions must be quick, since the price of delay or panic is the life of the child.
Open fractures pose a threat of infection, so a mandatory condition for providing first aid to the victim is the administration of anti-tetanus serum. Treatment of fractures in children is usually carried out on an outpatient basis; hospitalization is required only if surgical reposition of the fragments is necessary.
The most common factors associated with fractures in children and adolescents are:
- lack of calcium in the body - this microelement is the most basic “building material” of bone tissue;
- unbalanced nutrition - for the full growth and development of the musculoskeletal system in children, they need proteins, microelements and vitamins, as a rule, all these components are contained in those foods that children do not like or eat in small quantities;
- insufficiently active lifestyle - modern teenagers and children prefer to spend their holidays playing computer games rather than in the fresh air, playing and playing sports;
- hormonal changes in the body - fractures in adolescents often coincide with a rapid growth spurt.
To avoid injuries and fractures in children and adolescents, parents should pay special attention to their lifestyle, nutrition and health status, leading by example.
In order to increase the strength of bones and the musculoskeletal system as a whole, you need to follow simple tips:
- eat a full and balanced diet - if you do not know what is included in a balanced diet, seek help from a nutritionist or pediatrician;
- lead an active and mobile lifestyle;
- spend more time in the fresh air;
- During the period of intensive growth, do not overload the musculoskeletal system with increased physical activity.
source
Bone fractures in children occur not only because of pampering; sometimes the fragility of bone tissue is to blame. Why does it occur, how to detect and treat it?
Our expert is pediatrician Anna Mikhailova.
Experts call this condition osteopenia, which means that bone mineral density is below normal. According to various studies, disorders of this kind are found in every third teenager aged 11–17 years.
There are four main risk factors:
Deficiency of calcium, the main “building material” for bone tissue.
Poor nutrition. In addition to calcium, bones need protein, phosphorus, iron, copper, zinc and manganese, vitamins (from autumn to summer it is necessary to take vitamin-mineral complexes). And all these beneficial substances, as a rule, are present in those foods that children like least.
Physical inactivity – to build bone mass, movement is necessary that loads and trains the bones.
“Hormonal storm”: calcium metabolism in the body is under strict control of the hormonal system, and during puberty, disruptions in its functioning are common.
The normal absorption of calcium is also “interfered” with many chronic diseases: gastrointestinal tract, respiratory tract, liver, kidneys, thyroid gland...
Loss of bone density develops slowly and gradually, it is impossible to notice it by eye. But there are five indirect signs that should alert parents.
The child's cases of caries have become more frequent.
“For some reason,” hair splits, nails peel and break.
From time to time there is pain in the legs, especially in the legs.
The student is slouching more and more, his back gets tired after sitting for a long time at homework or at the computer.
Your child is allergic, because of this he has dietary restrictions; he does not eat dairy products or fish.
Even one such symptom is a signal that the child needs to be examined and find out whether he really does not have enough calcium.
First of all, the pediatrician will prescribe biochemical tests of blood and urine, which can be used to determine whether phosphorus-calcium metabolism is impaired. These partner minerals are involved in many vital metabolic processes and work hand in hand: the body cannot absorb calcium if there is not enough phosphorus, but if there is an excess of the latter, calcium is excreted from the body. That's why it's so important to maintain their balance. By comparing the data with the standard indicators for a certain age and detecting deviations, one can suspect the initial stage of osteopenia.
To clarify the diagnosis, densitometry is performed: assessment of bone tissue (ultrasound is often used). Unlike adults, children are analyzed only by the so-called Z-criterion - that is, deviations from the norm in indicators depending on the age and gender of the young patient, which are calculated using a special computer program.
The process of formation of healthy bone tissue can be adjusted as the child grows. For treatment, medications containing calcium are prescribed.
There is a wide choice: for example, for the sake of prevention and in case of minor deviations from the norm, calcium supplements with vitamin D are prescribed. If a deficiency of not only calcium, but also some microelements is detected, complex preparations are used (they also include
manganese, boron, copper, zinc, magnesium).
Since the absorption of calcium is affected by some chronic diseases, children who have them are selected with special drugs, for example, for gastritis with high acidity, those that “protect” the process of its absorption from the aggression of gastric juice. The course of continued treatment is individual.
But medication alone is not enough. Treatment should be supported by a diet: cottage cheese, cheese, kefir or yoghurt, fish (salmon, sardines), meat, eggs, broccoli, bananas, and legume dishes are recommended.
And of course, you need to make time for sports: at least for regular visits to the pool or fitness room. Precisely regular, not occasionally. And if a child has poor posture or flat feet, it is necessary to undergo treatment under the supervision of a pediatric orthopedic surgeon.
source
Almost every child, and therefore his parents, faces the problem of a fracture sooner or later. In order to correctly assess the severity of the situation and seek qualified help in time, you should be aware of the characteristics of fractures in children. Parents often underestimate the severity of the condition because some children are not very sensitive to pain; Some adults consider this almost the norm, explaining it by the child’s mobility. Is it that simple?
As is known from medical statistics, fractures in children account for about 15% of all injuries and injuries for which they seek qualified medical help. The problem is due to the peculiarity of the structure of the human body: the biological mechanics, anatomy and even physiology of a minor are very different from those inherent in an adult, since the body is actively growing and developing. Injuries accompanied by fractures, including violation of the integrity of the epiphysis, are an urgent problem of modern medicine. Updated approaches to refined diagnostics are being developed, and treatment strategies are being formed that would fully satisfy the characteristics of the case.
The key feature of fractures in children is the structure of bone tissue. The musculoskeletal system contains not only a fairly large amount of cartilage tissue, but is also distinguished by the presence of endplates, which an adult does not normally have. Such areas are called growth areas. Children's bones are characterized by increased strength and have a reliable periosteum, which forms callus in a short time. Biomechanical studies have shown the ability to absorb large amounts of energy. Scientists explained this by the porosity of the elements and low mineral density. The abundance of pores in bone tissue is associated with numerous large Haversian canals, due to which the elastic modulus decreases and strength decreases. Growth and maturation are accompanied by a decrease in porosity and thickening of the cortical block, which makes the skeletal system stronger.
Another feature of fractures in children is due to the attachment of ligamentous blocks to the bone epiphyses. Consequently, trauma to the limb can damage the growth site of the bone. The strength of the elements is ensured by the interweaving of annular blocks and mastoid bodies, but in any case, the growth area is characterized by relatively low strength. This is noticeable if we compare the anatomical features and qualities of the metaphysis, ligamentous fibers, and growth zones. Such areas are relatively resistant to tension, but are subject to the negative influence of torsional force. It is known from statistics that violation of the integrity of the growth plate is most often explained by angular influence or rotation.
Another feature of a fracture in children is the possibility of a displaced format, and the probability directly depends on the quality and parameters of the periosteum. The thicker this block, the lower the risk of closed reduction. After changing the position, it is she who is responsible for maintaining the fragments in the correct and stable state.
Fractures in children are accompanied by bone remodeling. The process is ensured by resorption of the periosteum, accompanied by the generation of new bone tissue. Anatomical reduction is needed only in a limited number of cases. Many traumatized children do not need such an intervention at all. The regeneration process depends on several factors: age, location of the injury relative to the joint, and the presence of obstacles to its activity. Remodeling is determined by the potential ability of the bone to grow, and the lower the age, the greater the potential.
If the injury is localized near the growth block, recovery will require minimal time, especially when the deformity coincides with the articular axis of movement. An intra-articular fracture, in which areas have shifted, heals more slowly. Restoration of the diaphysis requires considerable time. Possible rotational injury or leading to deterioration of joint motility. These heal slower than others.
One of the characteristics of bone fractures in children is the risk of excessive bone growth. Regarding long bones, this is explained by the effect on growth areas - in this area, blood flow is activated, which is necessary for the restoration of damaged tissue. It is noted that a fracture of the femur in a child under ten years of age is often accompanied by lengthening of the bone by several centimeters in the next couple of years. To minimize the undesirable consequences of rehabilitation, it is necessary to combine bone fragments in a bayonet-like manner. For patients older than this age, excessive development is less dangerous, the process is relatively weakly expressed. If a fracture occurs, it is necessary to provide assistance by simply repositioning the blocks.
A feature of bone fractures in children known to doctors is the progression of deformation. Sometimes the injury is accompanied by damage to the pineal gland. As a result, the site may be closed by a few percent or completely. This leads to angular deformation and can cause shortening of the bone element. There is a possibility of both types of complications. The level of deformation depends on the specifics of the bone and is determined by the ability of the bone tissue to grow.
Studies have shown that fractures in children heal faster than in adult trauma patients. The reason for this is the ability of the child’s skeletal system to quickly grow and increase the thickness of individual blocks. The juvenile periosteum is the area of localization of active metabolic processes. The older the person, the lower the healing rate.
Sooner or later, bone fractures in children become a problem for almost any family. The more restless the child, the higher the risk of serious injury. Parents must be aware of the manifestations of the problem and know how to provide first aid to the victim. In many ways, the speed and quality of the rehabilitation period depend on it. They determine what kind of help is needed at first, based on the cause of the fracture and factors that determine the specifics of the situation. However, the general tactics are the same for all cases.
From statistical observations it is known that the most common concern is a broken arm in a child; the incidence rate of foot fractures is half as high. If the injury is severe, it is immediately clear what happened, but more often children suffer minor injuries, and only a qualified doctor can diagnose correctly. Some do not pay enough attention to the situation, since the functionality of the affected limb, although impaired, is weak. You can easily confuse a fracture, a bruise, a dislocation. The first in the upper extremities are most often localized in the area of the forearm and elbow joint.
If a fracture in a child (arm, leg or other part of the body) is observed in this form, it is necessary to give the victim rest and ensure immobility. This step is the first in providing emergency care immediately after an injury. Parents should put the patient to bed, then calm down, since chaotic panic actions will only harm the baby. A cold compress is applied to the affected area. This provides relief and helps reduce internal bleeding. The next stage is immobilization. The term refers to measures to prevent movement of the affected area. The limb must be kept elevated. The patient is then given an analgesic. Doctors recommend using medications containing ibuprofen and paracetamol. Other medications are prohibited until the doctor arrives.
Treatment of open fractures in children should be left to a doctor. The task of those near the victim is to provide first aid. A distinctive feature of the injury is an open wound, which means it needs to be treated as quickly as possible and prevent large-scale blood loss. To stop bleeding, the damaged area is covered with a thick bandage. If the area is dirty, clean it with soapy water. Next, a cold compress is applied, the victim is kept immobile, and an analgesic is given if necessary.
Taking into account the briefly described above features of bone fractures in children, the importance of providing correct first aid becomes clear, since unsuccessful measures and the lack of suitable treatment can negatively affect a person’s future, lead to skeletal asymmetry and other complications. The key relief measure is immobilization of the affected area. To do this, apply a splint. Any car owner's first aid kit is equipped with such a product. It must be at the disposal of the ambulance team. Parents, when providing first aid to an injured child, should prepare a splint from available materials. Finding something suitable is not difficult - just use a dense material to which the injured part of the body is attached.
As with a displaced fracture in a child, and without such a complication, the task of first aid providers is to find suitable means for immobilization. You can use thick cardboard or plywood. If you have a small board or stick on hand, these items will also work. If a very small baby is injured, it is better to use cardboard and wrap it in cotton wool. A bandage is used to fix the diseased area. It is necessary to stabilize the position of the joints above and below the affected area. There is no need to take off clothes or shoes. It is advisable to take wide objects for applying a splint - they are more reliable than narrow ones. If a limb is injured, it is necessary to fix it in its current position, without adjusting it to a more familiar one or one that seems comfortable or correct from the outside. It is strictly prohibited to adjust the affected block of the support system - this will be done by a doctor.
If a displaced fracture occurs in a child, if the injury is not accompanied by displacement, it is necessary to call a doctor as soon as possible. If the situation occurred when the family was in a populated area where it is possible to call an ambulance, the limb may not be immobilized. Parents need to urgently seek medical support, and while waiting for the car with doctors, guarantee the victim peace and immobility. Do not touch the sore area.
There is a situation when a child is injured, but the elders do not have anything suitable for applying a splint at hand. You need to tape the painful area to a healthy part of the body.
One of the features of the treatment of fractures in children is a strict ban on heating and rubbing the affected area. Parents must monitor the behavior of the victim: he must not move. Under no circumstances should the injured person be forced to move or encouraged to move. It would be dangerous to try to correct the zone on your own. Do not treat the area with gels or ointments.
The rules for providing primary care for both upper and lower extremity injuries are almost the same. If your hand is injured, you should additionally secure it with a scarf. If the injury is localized in the leg, such measures are not required. If damage to the femur or injury involving the pelvic blocks is suspected, four joints are immobilized instead of two.
Doctors, finding out the characteristics of fractures in children and adults, have found that when equal force is applied, an older person is more likely to be injured than a child. The support system in childhood is highly elastic, and its forming elements are flexible. To some extent, a fracture is similar to a broken tree branch. The fragments do not move, which means regeneration requires minimal time. The most difficult case to clarify is if the fracture is localized in the growth area. When examining a part of the body using X-rays, it is impossible to see the cartilage tissue, so identifying the fracture is problematic.
The high regenerative abilities inherent in the children's body are known. The callus is quickly replaced by the corresponding tissue. Comparing the characteristics of fractures in children and adults, it was found that in the former, areas of scarring appear much less frequently. It was found that in children who have received a fracture, it is possible to maintain an insignificant displacement - it will disappear on its own as the body grows.
It is customary to divide all cases into pathological and caused by trauma. The latter are usually observed in everyday life. In a child, fractures of the collarbone, limbs, and other parts of the body are provoked by blows, falls, and jumps. They are not uncommon during games and can be explained by twisting a leg or running for a long time. Pathological cases are provoked by diseases. These are observed in dysplasia, bone tuberculosis, and may indicate improper formation of bone tissue at the embryonic stage of development. A possible cause is a lack of calcium. Sometimes a fracture indicates an inflammatory process localized in the bone tissue.
All cases of injury are divided into open and closed (the general rules of first aid are discussed above). The dangers of the open form should not be underestimated, since damage to the skin is accompanied by the danger of infection of the body. In a child, a fracture of the collarbone, limb, rib or any other block of the support system is accompanied by ruptures, and the dimensions of the damage vary from case to case. Sometimes they are small, in others they are large, leading to the destruction of soft tissue. In addition to introducing dirt, there is a danger of crushing tissue. Cases of open fracture are divided into those accompanied by displacement and those without it. The first involves the movement of bone fragments to the sides, the second option is characterized by a stable position of the fragments in their original location. Fractures with displacement can be incomplete or complete. The connection of the fragments is partially broken, while the bone integrity is preserved - these are features of an incomplete fracture. The second option involves complete separation of the elements.
The main percentage of cases are isolated injuries, in which one segment is damaged. Less common are multiple, combined cases affecting several areas of the body.
The task of parents is to know the symptoms of a fracture in a child in order to call a doctor in time and provide first aid. There are general signs inherent in any injury of this type, regardless of location. All manifestations are divided into probable and reliable. The first category includes skin swelling, hematoma, pain accompanying movement, and palpation. The mobility of the hand, foot, and finger is impaired. Reliable manifestations include deformation of the area and crepitus. The term refers to a crunching sound heard due to the appearance of bone fragments.
Not long ago, the medical community became interested in the case of a child who often suffered from fractures. In just a couple of years, the seven-year-old child received three fractures of the upper extremities, which were not accompanied by preliminary pressure. Doctors were unable to find any prerequisites for bone fragility; the patient ate well and led an active life. Laboratory studies showed adequate concentrations of trace elements and minerals in the blood. The only questionable result of the study was the level of antibodies, allowing one to suspect celiac disease. The diagnosis was confirmed by gastroenterologists.
As studies have proven, a child is more likely to have fractures of the radius, collarbone and other parts of the body due to celiac disease than in the absence of this disease, since it affects mineral density. An interesting, reliable study was organized in 2011. It turned out that about a quarter of all people diagnosed with celiac disease had recently suffered a fracture.
Celiac disease is a pathological condition in which the functioning of the intestinal villi is impaired. The absorption function of the tract is inhibited, the body does not receive the necessary components. This leads to deficiency of iron, vitamin compounds, and folic acid. One of the features of fractures of tubular bones in children (as well as any other elements of the supporting system) is low density, which is caused by a lack of nutrients. Accordingly, celiac disease leads to decreased bone strength. In parallel, the level of inflammation increases, which also negatively affects the health of the supporting system.
Finding out the characteristics of fractures in children's jaws, limbs and other parts of the body due to celiac disease, doctors considered that the only reliable method of prevention is proper nutrition. It is necessary to completely eliminate gluten from the patient’s diet. As the researchers of the above-mentioned case noted, this measure applied to the child made it possible to avoid fractures for the next 3.5 years (exactly after the parents brought the child to the clinic for a preventive examination). It is noted that adjustment to a new nutrition system is not easy for children, but the results are worth it.
If we do not touch on the topic of rare congenital and hereditary diseases, we will have to admit: the main percentage of fractures in minors is due to industrial society and the characteristics of social interaction. It is not easy for children to learn to follow household rules and behave correctly in transport, which means that the risk of injury increases. Doctors involved in the diagnosis and treatment of fractures in children note: about 70% of all cases are caused by riding bicycles, skateboards, scooters, and rollerblades. Many children ride where it is prohibited, jump in dangerous places, and fall. Even vehicles do not cause injury to minors as often as occurs due to domestic reasons. On average, the likelihood of injury due to transport is higher for an adult than for a child, but the severity of injury usually dominates in the latter. Studies have shown that on average per thousand children there are 248 people with bruises, 30 with dislocations and about 57 with bone fractures.
To understand how to distinguish these cases, it is necessary to consider their features, at least in general terms.
A bruise is a closed injury in which organs and tissues suffer, but the structure remains intact. The sections do not come off or rupture, but the integrity of the blood vessels may be damaged. The result is hematomas and bruises. Bruises are visually visible as purple spots, the shade of which gradually transforms to green and yellow. Usually the cause is a collision, fall, blow. The mobility of the diseased part of the body is preserved, but the area responds with pain. To help the victim, apply a cold compress to the area and provide rest.
As studies show, it is possible for an infant to get a fracture, but ligament sprains appear only in people over the age of three. The classic location is the ankle joint. The child makes an awkward movement, the foot turns under. This is possible when a person runs or walks. The risk is especially high when running up stairs. A sprain is indicated by acute pain, followed by possible swelling of the affected area. The skin tone sometimes changes to bluish, and palpation causes pain. Movements in the joint are possible, but the victim tries to spare the affected limb, so he practically does not lean on it.
Parents should apply ice to the affected area, secure it with an elastic bandage, and show the injured person to the doctor for an x-ray examination. There is a high risk of a bone fracture, with symptoms similar to a sprain. X-ray is the only way to clarify the condition.
The word refers to an injury in which the articular contour is disrupted. Most often the reason is a fall. Movement of the diseased area is limited, pain becomes stronger, and the ability to move is inhibited. The limb injured by the fall becomes longer or shorter than the limb. There is a possibility of deformation.
Parents should provide the patient with rest and secure the affected area with a splint or bandage. It is necessary to seek help from a qualified doctor. You can't fix a dislocation on your own.
Subluxation is very common in practice, with the elbow joint being a typical area. This is most often observed in children aged from one to three years. An adult holds the child's hand tightly, but the child stumbles, suddenly slips or falls, and this leads to injury. The moment is sometimes accompanied by a specific crunch.
With subluxation, the affected area responds with pain, the child does not move the limb, stretches it along the body, sometimes bends it slightly. If you rotate your forearm or elbow, the pain becomes especially severe. Parents should ensure peace in the affected area and take the patient to a pediatric traumatology department.
When considering the characteristics of bone fractures in newborns, infants, and older children, one cannot ignore cracks. This term refers to partial damage to bone tissue, a fracture that is not completed. It is not easy to identify him, since young children are unable to formulate complaints. From the outside, there is a general concern of the child. The risk of injury is especially high due to the child's light weight. If a child falls, the soft tissue somewhat weakens the aggressive influence, so the likelihood of a crack occurring is greater than a fracture.
An older child can describe the manifestations of the situation. The injured area is bothered by pain, especially severe during movement, palpation, and pressure. If you provide rest to the affected area, the pain dulls, the area pulsates, and in some it tingles. The tissues swell, and the symptom can progress quickly. The swelling will subside a day after the crack occurs or later. Often the area is marked with a hematoma. The victim's limited mobility is noticeable, which is explained by pain and swelling.
A relatively common diagnosis is a compression fracture. In a child (as well as an adult), this is due to compression of the elements of the spinal column. This is possible when falling, due to a blow to the back, somersault, or gymnastic practice. It is known that in children, muscles are sometimes stronger than the skeletal system. When they contract intensively, a compression effect is formed, affecting individual blocks of the column in the lateral projection. Functionality and sensitivity are not impaired, since there is no spinal injury, but the structure of the column is impaired. The clinical symptoms of the condition are often vague. At the moment of injury, the child catches his breath, the back gives off slight pain, while the child does not even pay attention to the manifestations and continues his games and activities.
Without adequate treatment, a compression fracture leads to complications. These are more common after years. The consequences of the situation include radiculitis, osteochondrosis, vertebral destruction and other similar pathological processes. To prevent the consequences, it is necessary to take the victim to the trauma department of the clinic at the slightest back injury, where they will take an X-ray, assess the danger of the condition and select a therapeutic program. Inpatient treatment is often indicated. Rehabilitation is accompanied by a special daily routine aimed at unloading the spinal column. This treatment takes quite a long time.
To correct a compression fracture, it is necessary to do therapeutic exercises. Swimming is recommended from the age of three. Without adequate support from the body, as you get older and gain weight, the risk of a hernia in the affected area increases.
Almost every child, and therefore his parents, faces the problem of a fracture sooner or later. In order to correctly assess the severity of the situation and seek qualified help in time, you should be aware of the characteristics of fractures in children. Parents often underestimate the severity of the condition because some children are not very sensitive to pain; Some adults consider this almost the norm, explaining it by the child’s mobility. Is it that simple?
Relevance of the issue
As is known from medical statistics, fractures in children account for about 15% of all injuries and injuries for which they seek qualified medical help. The problem is due to the peculiarity of the structure of the human body: the biological mechanics, anatomy and even physiology of a minor are very different from those inherent in an adult, since the body is actively growing and developing. Injuries accompanied by fractures, including violation of the integrity of the epiphysis, are an urgent problem of modern medicine. Updated approaches to refined diagnostics are being developed, and treatment strategies are being formed that would fully satisfy the characteristics of the case.
A key feature of fractures in children is the structure of bone tissue. The musculoskeletal system contains not only a fairly large amount of cartilage tissue, but is also distinguished by the presence of endplates, which an adult does not normally have. Such areas are called growth areas. Children's bones are characterized by increased strength and have a reliable periosteum, which forms callus in a short time. Biomechanical studies have shown the ability to absorb large amounts of energy. Scientists explained this by the porosity of the elements and low mineral density. The abundance of pores in bone tissue is associated with numerous large Haversian canals, due to which the elastic modulus decreases and strength decreases. Growth and maturation are accompanied by a decrease in porosity and thickening of the cortical block, which makes the skeletal system stronger.
Anatomy and injuries
Another feature of fractures in children is due to the attachment of ligamentous blocks to the bone epiphyses. Consequently, trauma to the limb can damage the growth site of the bone. The strength of the elements is ensured by the interweaving of annular blocks and mastoid bodies, but in any case, the growth area is characterized by relatively low strength. This is noticeable if we compare the anatomical features and qualities of the metaphysis, ligamentous fibers, and growth zones. Such areas are relatively resistant to tension, but are subject to the negative influence of torsional force. It is known from statistics that violation of the integrity of the growth plate is most often explained by angular influence or rotation.
Another feature of a fracture in children is the possibility of a displaced format, and the probability directly depends on the quality and parameters of the periosteum. The thicker this block, the lower the risk of closed reduction. After changing the position, it is she who is responsible for maintaining the fragments in the correct and stable state.
Healing process
Fractures in children are accompanied by bone remodeling. The process is ensured by resorption of the periosteum, accompanied by the generation of new bone tissue. Anatomical reduction is needed only in a limited number of cases. Many traumatized children do not need such an intervention at all. The regeneration process depends on several factors: age, location of the injury relative to the joint, and the presence of obstacles to its activity. Remodeling is determined by the potential ability of the bone to grow, and the lower the age, the greater the potential.
If the injury is localized near the growth block, recovery will require minimal time, especially when the deformity coincides with the articular axis of movement. in which areas have shifted, it overgrows more slowly. Restoration of the diaphysis requires considerable time. Possible rotational injury or leading to deterioration of joint motility. These heal slower than others.
Bones: are they growing in moderation?
One of the features of bone fractures in children is the risk of excessive bone growth. Regarding long bones, this is explained by the effect on growth areas - in this area, blood flow is activated, which is necessary for the restoration of damaged tissue. It is noted that a fracture of the femur in a child under ten years of age is often accompanied by lengthening of the bone by several centimeters in the next couple of years. To minimize the undesirable consequences of rehabilitation, it is necessary to combine bone fragments in a bayonet-like manner. For patients older than this age, excessive development is less dangerous, the process is relatively weakly expressed. If a fracture occurs, it is necessary to provide assistance by simply repositioning the blocks.
About the nuances
A feature of bone fractures in children known to doctors is the progression of deformation. Sometimes the injury is accompanied by damage to the pineal gland. As a result, the site may be closed by a few percent or completely. This leads to angular deformation and can cause shortening of the bone element. There is a possibility of both types of complications. The level of deformation depends on the specifics of the bone and is determined by the ability of the bone tissue to grow.
Studies have shown that fractures in children heal faster than in adult trauma patients. The reason for this is the ability of the child’s skeletal system to quickly grow and increase the thickness of individual blocks. The juvenile periosteum is the area of localization of active metabolic processes. The older the person, the lower the healing rate.
Do you need help?
Sooner or later, bone fractures in children become a problem for almost any family. The more restless the child, the higher the risk of serious injury. Parents must be aware of the manifestations of the problem and know how to provide first aid to the victim. In many ways, the speed and quality of the rehabilitation period depend on it. They determine what kind of help is needed at first, based on the cause of the fracture and factors that determine the specifics of the situation. However, the general tactics are the same for all cases.
From statistical observations it is known that the most common concern is a broken arm in a child; the incidence rate of foot fractures is half as high. If the injury is severe, it is immediately clear what happened, but more often children suffer minor injuries, and only a qualified doctor can diagnose correctly. Some do not pay enough attention to the situation, since the functionality of the affected limb, although impaired, is weak. You can easily confuse a fracture, a bruise, a dislocation. The first in the upper extremities are most often localized in the area of the forearm and elbow joint.
Closed fracture
If a fracture in a child (arm, leg or other part of the body) is observed in this form, it is necessary to give the victim rest and ensure immobility. This step is the first in providing emergency care immediately after an injury. Parents should put the patient to bed, then calm down, since chaotic panic actions will only harm the baby. A cold compress is applied to the affected area. This provides relief and helps reduce internal bleeding. The next stage is immobilization. The term refers to measures to prevent movement of the affected area. The limb must be kept elevated. The patient is then given an analgesic. Doctors recommend using medications containing ibuprofen and paracetamol. Other medications are prohibited until the doctor arrives.
Open fracture
Treatment of open fractures in children should be left to a doctor. The task of those near the victim is to provide first aid. A distinctive feature of the injury is an open wound, which means it needs to be treated as quickly as possible and prevent large-scale blood loss. To stop bleeding, the damaged area is covered with a thick bandage. If the area is dirty, clean it with soapy water. Next, a cold compress is applied, the victim is kept immobile, and an analgesic is given if necessary.

About committing
Taking into account the briefly described above features of bone fractures in children, the importance of providing correct first aid becomes clear, since unsuccessful measures and the lack of suitable treatment can negatively affect a person’s future, lead to skeletal asymmetry and other complications. The key relief measure is immobilization of the affected area. To do this, apply a splint. Any car owner's first aid kit is equipped with such a product. It must be at the disposal of the ambulance team. Parents, when providing first aid to an injured child, should prepare a splint from available materials. Finding something suitable is not difficult - just use a dense material to which the injured part of the body is attached.
As with a displaced fracture in a child, and without such a complication, the task of first aid providers is to find suitable means for immobilization. You can use thick cardboard or plywood. If you have a small board or stick on hand, these items will also work. If a very small baby is injured, it is better to use cardboard and wrap it in cotton wool. A bandage is used to fix the diseased area. It is necessary to stabilize the position of the joints above and below the affected area. There is no need to take off clothes or shoes. It is advisable to take wide objects for applying a splint - they are more reliable than narrow ones. If a limb is injured, it is necessary to fix it in its current position, without adjusting it to a more familiar one or one that seems comfortable or correct from the outside. It is strictly prohibited to adjust the affected block of the support system - this will be done by a doctor.
First aid: nuances
If a displaced fracture occurs in a child, if the injury is not accompanied by displacement, it is necessary to call a doctor as soon as possible. If the situation occurred when the family was in a populated area where it is possible to call an ambulance, the limb may not be immobilized. Parents need to urgently seek medical support, and while waiting for the car with doctors, guarantee the victim peace and immobility. Do not touch the sore area.
There is a situation when a child is injured, but the elders do not have anything suitable for applying a splint at hand. You need to tape the painful area to a healthy part of the body.
Strictly prohibited
One of the features of the treatment of fractures in children is a strict ban on heating and rubbing the diseased area. Parents must monitor the behavior of the victim: he must not move. Under no circumstances should the injured person be forced to move or encouraged to move. It would be dangerous to try to correct the zone on your own. Do not treat the area with gels or ointments.
The rules for providing primary care for both upper and lower extremity injuries are almost the same. If your hand is injured, you should additionally secure it with a scarf. If the injury is localized in the leg, such measures are not required. If damage to the femur or injury involving the pelvic blocks is suspected, four joints are immobilized instead of two.

Subtleties of the question
Doctors, finding out the characteristics of fractures in children and adults, have found that when equal force is applied, an older person is more likely to be injured than a child. The support system in childhood is highly elastic, and its forming elements are flexible. To some extent, a fracture is similar to a broken tree branch. The fragments do not move, which means regeneration requires minimal time. The most difficult case to clarify is if the fracture is localized in the growth area. When examining a part of the body using X-rays, it is impossible to see the cartilage tissue, so identifying the fracture is problematic.
The high regenerative abilities inherent in the children's body are known. The callus is quickly replaced by the corresponding tissue. Comparing the characteristics of fractures in children and adults, it was found that in the former, areas of scarring appear much less frequently. It was found that in children who have received a fracture, it is possible to maintain an insignificant displacement - it will disappear on its own as the body grows.
Fractures: forms
It is customary to divide all cases into pathological and caused by trauma. The latter are usually observed in everyday life. In a child, fractures of the collarbone, limbs, and other parts of the body are provoked by blows, falls, and jumps. They are not uncommon during games and can be explained by twisting a leg or running for a long time. Pathological cases are provoked by diseases. These are observed in dysplasia, bone tuberculosis, and may indicate improper formation of bone tissue at the embryonic stage of development. A possible reason is a lack of calcium. Sometimes a fracture indicates an inflammatory process localized in the bone tissue.
All cases of injury are divided into open and closed (the general rules of first aid are discussed above). The dangers of the open form should not be underestimated, since damage to the skin is accompanied by the danger of infection of the body. In a child, a fracture of the collarbone, limb, rib or any other block of the support system is accompanied by ruptures, and the dimensions of the damage vary from case to case. Sometimes they are small, in others they are large, leading to the destruction of soft tissue. In addition to introducing dirt, there is a danger of crushing tissue. Cases of open fracture are divided into those accompanied by displacement and those without it. The first involves the movement of bone fragments to the sides, the second option is characterized by a stable position of the fragments in their original location. Fractures with displacement can be incomplete or complete. The connection of the fragments is partially broken, while the bone integrity is preserved - these are features of an incomplete fracture. The second option involves complete separation of the elements.
The main percentage of cases are isolated injuries, in which one segment is damaged. Less common are multiple, combined cases affecting several areas of the body.

How to notice?
The task of parents is to know the symptoms of a fracture in a child in order to call a doctor in time and provide first aid. There are general signs inherent in any injury of this type, regardless of location. All manifestations are divided into probable and reliable. The first category includes skin swelling, hematoma, pain accompanying movement, and palpation. The mobility of the hand, foot, and finger is impaired. Reliable manifestations include deformation of the area and crepitus. The term refers to a crunching sound heard due to the appearance of bone fragments.
This is interesting: trauma and celiac disease
Not long ago, the medical community became interested in the case of a child who often suffered from fractures. In just a couple of years, the seven-year-old child received three fractures of the upper extremities, which were not accompanied by preliminary pressure. Doctors were unable to find any prerequisites for bone fragility; the patient ate well and led an active life. Laboratory studies showed adequate concentrations of trace elements and minerals in the blood. The only questionable result of the study was the level of antibodies, allowing one to suspect celiac disease. The diagnosis was confirmed by gastroenterologists.
As studies have proven, a child is more likely to have fractures of the radius, collarbone and other parts of the body due to celiac disease than in the absence of this disease, since it affects mineral density. An interesting, reliable study was organized in 2011. It turned out that about a quarter of all people diagnosed with celiac disease had recently suffered a fracture.
Why is this happening?
Celiac disease is a pathological condition in which the functioning of the intestinal villi is impaired. The absorption function of the tract is inhibited, the body does not receive the necessary components. This leads to deficiency of iron, vitamin compounds, and folic acid. One of the features of fractures of tubular bones in children (as well as any other elements of the supporting system) is low density, which is caused by a lack of nutrients. Accordingly, celiac disease leads to decreased bone strength. In parallel, the level of inflammation increases, which also negatively affects the health of the supporting system.
Finding out the characteristics of fractures in children's jaws, limbs and other parts of the body against the background of celiac disease, doctors considered: the only reliable method of prevention is proper nutrition. It is necessary to completely eliminate gluten from the patient’s diet. As the researchers of the above-mentioned case noted, this measure applied to the child made it possible to avoid fractures for the next 3.5 years (exactly after the parents brought the child to the clinic for a preventive examination). It is noted that adjustment to a new nutrition system is not easy for children, but the results are worth it.

Causes and consequences
If we do not touch on the topic of rare congenital and hereditary diseases, we will have to admit: the main percentage of fractures in minors is due to industrial society and the characteristics of social interaction. It is not easy for children to learn to follow household rules and behave correctly in transport, which means that the risk of injury increases. Doctors involved in the diagnosis and treatment of fractures in children note: about 70% of all cases are caused by riding bicycles, skateboards, scooters, and rollerblades. Many children ride where it is prohibited, jump in dangerous places, and fall. Even vehicles do not cause injury to minors as often as occurs due to domestic reasons. On average, the likelihood of injury due to transport is higher for an adult than for a child, but the severity of injury usually dominates in the latter. Studies have shown that on average per thousand children there are 248 people with bruises, 30 with dislocations and about 57 with bone fractures.
To understand how to distinguish these cases, it is necessary to consider their features, at least in general terms.
About terms and situations
A bruise is a closed injury in which organs and tissues suffer, but the structure remains intact. The sections do not come off or rupture, but the integrity of the blood vessels may be damaged. The result is hematomas and bruises. Bruises are visually visible as purple spots, the shade of which gradually transforms to green and yellow. Usually the cause is a collision, fall, blow. The mobility of the diseased part of the body is preserved, but the area responds with pain. To help the victim, apply a cold compress to the area and provide rest.
As studies show, it is possible for an infant to get a fracture, but ligament sprains appear only in people over the age of three. The classic location is the ankle joint. The child makes an awkward movement, the foot turns under. This is possible when a person runs or walks. The risk is especially high when running up stairs. A sprain is indicated by acute pain, followed by possible swelling of the affected area. The skin tone sometimes changes to bluish, and palpation causes pain. Movements in the joint are possible, but the victim tries to spare the affected limb, so he practically does not lean on it.
Parents should apply ice to the affected area, secure it with an elastic bandage, and show the injured person to the doctor for an x-ray examination. There is a high risk of a bone fracture, with symptoms similar to a sprain. X-ray is the only way to clarify the condition.

Dislocation: what is it?
The word refers to an injury in which the articular contour is disrupted. More often the reason is a fall. Movement of the diseased area is limited, pain becomes stronger, and the ability to move is inhibited. The limb injured by the fall becomes longer or shorter than the limb. There is a possibility of deformation.
Parents should provide the patient with rest and secure the affected area with a splint or bandage. It is necessary to seek help from a qualified doctor. You can't fix a dislocation on your own.
Subluxation is very common in practice, with the elbow joint being a typical area. This is most often observed in children aged from one to three years. An adult holds the child's hand tightly, but the child stumbles, suddenly slips or falls, and this leads to injury. The moment is sometimes accompanied by a specific crunch.
With subluxation, the affected area responds with pain, the child does not move the limb, stretches it along the body, sometimes bends it slightly. If you rotate your forearm or elbow, the pain becomes especially severe. Parents should ensure peace in the affected area and take the patient to a pediatric traumatology department.
Crack
When considering the characteristics of bone fractures in newborns, infants, and older children, one cannot ignore cracks. This term refers to partial damage to bone tissue, a fracture that is not completed. It is not easy to identify him, since young children are unable to formulate complaints. From the outside, there is a general concern of the child. The risk of injury is especially high due to the child's light weight. If a child falls, the soft tissue somewhat weakens the aggressive influence, so the likelihood of a crack occurring is greater than a fracture.
An older child can describe the manifestations of the situation. The injured area is bothered by pain, especially severe during movement, palpation, and pressure. If you provide rest to the affected area, the pain dulls, the area pulsates, and in some it tingles. The tissues swell, and the symptom can progress quickly. The swelling will subside a day after the crack occurs or later. Often the area is marked with a hematoma. The victim's limited mobility is noticeable, which is explained by pain and swelling.

The spine suffers
A relatively common diagnosis is a compression fracture. In a child (as well as an adult), this is due to compression of the elements of the spinal column. This is possible when falling, due to a blow to the back, somersault, or gymnastic practice. It is known that in children, muscles are sometimes stronger than the skeletal system. When they contract intensively, a compression effect is formed, affecting individual blocks of the column in the lateral projection. Functionality and sensitivity are not impaired, since there is no spinal injury, but the structure of the column is impaired. The clinical symptoms of the condition are often vague. At the moment of injury, the child catches his breath, the back gives off slight pain, while the child does not even pay attention to the manifestations and continues his games and activities.
Without adequate treatment, a compression fracture leads to complications. These are more common after years. The consequences of the situation include radiculitis, osteochondrosis, vertebral destruction and other similar pathological processes. To prevent the consequences, it is necessary to take the victim to the trauma department of the clinic at the slightest back injury, where they will take an X-ray, assess the danger of the condition and select a therapeutic program. Inpatient treatment is often indicated. Rehabilitation is accompanied by a special daily routine aimed at unloading the spinal column. This treatment takes quite a long time.
To correct a compression fracture, it is necessary to do therapeutic exercises. Swimming is recommended from the age of three. Without adequate support from the body, as you get older and gain weight, the risk of a hernia in the affected area increases.
A bone fracture in a child can be caused by injury, a fall, or a blow. Children are more active outside and at home. Because of this, frequent falls and blows are possible, as a result of which bone damage occurs. But children 1-2 years old are less susceptible to fractures than preschoolers. This is explained by the elasticity of the bones, which are not yet fully strengthened in children. Another reason why a child’s skeletal system may be damaged is serious injuries: a car accident, a fall from a height. With increased fragility of children's bones, damage occurs due to minor trauma.
Symptoms
- There is usually severe pain at the site of injury.
- A few hours after the injury, swelling appears in the damaged area of the body, and the pain begins to be aching in nature and spreads significantly beyond the site of injury.
- Gradually, the skin at the site of injury may become pale, and traces of damage are possible.
- In severe cases, there may be loss of pulse, tingling, numbness, and paralysis at or below the injury site.
- With a closed fracture, there will be no signs of damage on the surface of the skin.
- An open fracture can be recognized by the presence of bleeding and the appearance of a wound.
- If the first signs of a fracture are observed in different parts of the body, this may indicate multiple fractures.
- Multiple bone fractures in a child can be open or closed, along with the presence of corresponding signs.
Diagnosis of a bone fracture in a child
The presence of a bone fracture in a child can be determined after an initial examination and complaints from the victim at the emergency room or emergency department of a children's hospital. But in order to accurately diagnose bone damage, the doctor sends the baby for an X-ray examination. The damaged area is examined in two projections in order to most accurately determine the diagnosis and location of the damage. Sometimes MRI, CT and other diagnostic procedures may be prescribed. It happens that X-ray examination of children does not show the presence of a fracture. In this case, the procedure is repeated after 1-2 weeks. If an incomplete fracture or crack is suspected, a test using a tuning fork is prescribed. In severe cases, to determine the state of internal systems and organs, the child’s entire body is examined using tests and other procedures.
Complications
Typically, closed fractures heal within 1-2 months without causing complications. But in some cases, a fracture can be dangerous. With an open fracture, there may be poor circulation, blood loss, or blood poisoning through an open wound. If the spine is fractured, the child may subsequently develop osteochondrosis. In some cases, fractures cause spinal deformation and persistent pain. With a pelvic fracture, damage to the genitourinary system may occur.
Treatment
What can you do
If a fracture is suspected in a child, parents should provide first aid. You should not panic and you need to calm the baby. Before providing first aid, you must call the hospital and call an ambulance. For simple fractures, if possible, you can take the child to the nearest hospital yourself. It is necessary to use available means in the form of boards, sticks and other objects to immobilize the broken bone and secure it with a scarf, bandage or scarf. It is necessary to fix in a motionless position not only the bone with the fracture, but also the adjacent joints. If the pain is severe, the child can take a painkiller. With an open fracture, as a rule, damage to tissue and skin occurs. This may cause bleeding, which should be stopped as soon as possible. If there are means to disinfect the wound, it is necessary to disinfect it and apply a sterile bandage.
After the doctor examines and determines the type and severity of the fracture, proper care for the injured child is necessary. Parents should provide the baby with a balanced and nutritious diet, and also take care of the use of vitamin complexes.
What does a doctor do
For children under the age of 7 years, the main method of treating bone injuries without displacement is the application of a plaster splint to a part of the limb for up to 3-4 weeks. In simple cases of damage to children's bones, there is no need to be in the hospital. Treatment and recovery are usually carried out at home. The child must come to the doctor for examination once a week. If a child is diagnosed with a displaced fracture or severe comminuted bone damage, surgery using general anesthesia is necessary. After the necessary connections of the bones, a plaster splint is applied, and the baby remains in the hospital for several days. In some cases, fixation using metal pins or skeletal traction is used. After removing the plaster splint, the sick child can undergo a rehabilitation course of physiotherapy, massage, and physical therapy.
Prevention
It is necessary to explain to children the rules of safe behavior on the street, at home in child care institutions, and in transport. Young children require supervision. There should be no dangerous objects that could cause injury in the room where the child is located. Small children must be transported in a car using a special restraint device. Parents should feed their baby foods rich in calcium and phosphorus, as well as foods high in vitamins and minerals.
44386 0
The anatomical features of the structure of the skeletal system of children and its physiological properties determine the occurrence of certain types of fractures that are characteristic only of this age.
It is known that young children often fall during outdoor play, but they rarely experience bone fractures.
This is explained by the child’s lower body weight and well-developed soft tissue cover, and therefore by a weakening of the impact force during a fall.
Baby bones thinner and less durable, but more elastic than adult bones. Elasticity and flexibility depend on the smaller amount of mineral salts in the child’s bones, as well as on the structure of the periosteum, which in children is thicker and abundantly supplied with blood. The periosteum forms a kind of sheath around the bone, which gives it greater flexibility and protects it from injury.
The preservation of bone integrity is facilitated by the presence of epiphyses at the ends of the tubular bones, connected to the metaphyses by wide elastic growth cartilage, which weakens the force of impact. These anatomical features, on the one hand, prevent the occurrence of a bone fracture, on the other hand, in addition to the usual fractures observed in adults, they cause the following skeletal injuries typical for childhood: fractures, subperiosteal fractures, epiphysiolysis, osteoepiphysiolysis and apophysiolysis.
Breaks and fractures like a green branch or a willow twig are explained by the flexibility of bones in children.
This type of fracture is observed especially often when the diaphysis of the forearm is damaged. In this case, the bone is slightly bent, on the convex side the outer layers are subject to fracture, and on the concave side they retain their normal structure.
Subperiosteal fractures are characterized by the fact that the broken bone remains covered by the periosteum, the integrity of which is preserved. These injuries occur when force is applied along the longitudinal axis of the bone. Most often, subperiosteal fractures are observed on the forearm and lower leg; In such cases, bone displacement is absent or very insignificant.
Epiphysiolysis and osteoepiphysiolysis are traumatic separation and displacement of the epiphysis from the metaphysis or with part of the metaphysis along the line of the germinal epiphyseal cartilage.
They occur only in children and adolescents until the end of the ossification process (Fig. 14.1).
Epiphysiolysis occurs more often as a result of the direct action of force on the epiphysis and, according to the mechanism of injury, is similar to dislocations in adults, which are rarely observed in children. This is explained by the anatomical features of the bones and ligamentous apparatus of the joints, and the place of attachment of the articular capsule to the articular ends of the bone is of significant importance.
Epiphysiolysis and osteoepiphysiolysis are observed where the joint capsule is attached to the epiphyseal cartilage of the bone: for example, the wrist and ankle joints, the distal epiphysis of the femur. In places where the bursa is attached to the metaphysis so that the growth cartilage is covered by it and does not serve as a site of its attachment (for example, the hip joint), epiphysiolysis does not occur. This position is confirmed by the example of the knee joint.
Here, during injury, epiphysiolysis of the femur occurs, but there is no displacement of the proximal epiphysis of the tibia along the epiphyseal cartilage.
Apophysiolysis - separation of the apophysis along the line of the growth cartilage
Apophyses, unlike epiphyses, are located outside the joints, have a rough surface and serve for attachment of muscles and ligaments. An example of this type of injury would be displacement of the medial or lateral epicondyle of the humeral spine. With complete fractures of the bones of the extremities with displacement of bone fragments, the clinical manifestations are practically no different from those in adults.At the same time, with fractures, subperiosteal fractures, epiphysiolysis and osteoepiphysiolysis without displacement, movements can be preserved to a certain extent, pathological mobility is absent, the contours of the injured limb that the child is sparing remain unchanged and only upon palpation is pain determined in a limited area corresponding to the fracture site. In such cases, only x-ray examination helps to make the correct diagnosis.
A feature of bone fractures in a child is an increase in body temperature in the first days after injury from 37 to 38°C, which is associated with absorption of the contents of the hematoma.
In children, it is difficult to diagnose subperiosteal fractures, epiphysiolysis and osteoepiphysiolysis without displacement. Difficulty in establishing a diagnosis also arises with epiphysiolysis in newborns and infants, since even radiography does not always provide clarity due to the absence of ossification nuclei in the epiphyses.
In young children, most of the epiphysis consists of cartilage and is passable for x-rays, and the ossification nucleus gives a shadow in the form of a small dot. Only when compared with a healthy limb on radiographs in two projections is it possible to establish the displacement of the ossification nucleus in relation to the diaphysis of the bone.
Similar difficulties arise during birth epiphysiolysis of the heads of the humerus and femur, the distal epiphysis of the humerus, etc. At the same time, in older children, osteoepiphysiolysis without displacement is easier to diagnose, since radiographs show a separation of the bone fragment of the metaphysis of the tubular bone.
Errors in diagnosis are more often observed with fractures in young children. Insufficient medical history, well-defined subcutaneous tissue making palpation difficult, and the absence of displacement of fragments in subperiosteal fractures make recognition difficult. Often, in the presence of a fracture, a bruise is diagnosed.
As a result of improper treatment in such cases, curvature of the limb and impairment of its function are observed. In some cases, repeated X-ray examination, performed on the 7-10th day after injury, helps to clarify the diagnosis, which becomes possible due to the appearance of initial signs of fracture consolidation.
The leading principle is a conservative method of treatment (94%).
In most cases, a fixing bandage is applied. Immobilization is carried out with a plaster splint, usually in the mid-physiological position, covering 2/3 of the circumference of the limb and fixing two adjacent joints. A circular plaster cast is not used for fresh fractures in children, since there is a risk of circulatory disorders due to increasing edema with all the ensuing consequences (Volkmann’s ischemic contracture, bedsores and even necrosis of the limb).
During treatment, periodic x-ray monitoring (once a week) of the position of bone fragments is necessary, since secondary displacement of bone fragments is possible. Traction is used for fractures of the humerus, shin bones and mainly for fractures of the femur. Depending on the age, location and nature of the fracture, adhesive plaster or skeletal traction is used.
The latter is used in children over 3 years of age. Thanks to traction, displacement of the fragments is eliminated, gradual reposition is carried out and the bone fragments are held in the reduced position.
For bone fractures with displacement of fragments, one-stage closed reduction is recommended as early as possible after the injury.
In particularly difficult cases, reposition is performed under periodic X-ray control with radiation protection for the patient and medical personnel. Maximum shielding and minimal exposure allows for repositioning under visual control.
The choice of pain relief method is of no small importance.
Good anesthesia creates favorable conditions for reposition, since the comparison of fragments should be done in a gentle way with minimal tissue trauma. These requirements are met by anesthesia, which is widely used in hospital settings.
In outpatient practice, reposition is performed under local or regional anesthesia. Anesthesia is carried out by injecting a 1% or 2% novocaine solution into the hematoma at the fracture site (at the rate of 1 ml per one year of the child’s life). When choosing a treatment method for children and establishing indications for repeated closed or open reduction, the possibility of self-correction of some types of remaining displacements during growth is taken into account.
The degree of correction of the damaged limb segment depends both on the age of the child and on the location of the fracture, the degree and type of displacement of the fragments.
At the same time, if the growth zone is damaged (during epiphysiolysis), as the child grows, a deformation may appear that was not there during the treatment period, which should always be remembered when assessing the prognosis (Fig. 14.2). Spontaneous correction of the remaining deformity occurs the better, the younger the patient is.
The leveling of displaced bone fragments in newborns is especially pronounced.
In children under 7 years of age, displacements for diaphyseal fractures are allowed in the length range from 1 to 2 cm, in width - almost across the diameter of the bone and at an angle of no more than 10°. At the same time, rotational displacements cannot be corrected during growth and should be eliminated.
In children of the older age group, more accurate adaptation of bone fragments is necessary and it is necessary to eliminate deflections and rotational displacements. For intra- and periarticular fractures of the bones of the extremities, accurate reduction with the elimination of all types of displacement is required, since unresolved displacement of even a small bone fragment during an intra-articular fracture can lead to blockade of the joint or cause varus or valgus deviation of the limb axis.
Surgical intervention for bone fractures in children is indicated in the following cases:
1) for intra- and periarticular fractures with displacement and rotation of the bone fragment;
2) with two or three attempts at closed reduction, if the remaining displacement is classified as unacceptable;
3) with interposition of soft tissues between fragments;
4) with open fractures with significant damage to soft tissues;
5) in case of incorrectly healed fractures, if the remaining displacement threatens permanent deformation, curvature or stiffness of the joint;
6) for pathological fractures.
Open reduction is performed with special care, gentle surgical access, with minimal trauma to soft tissues and bone fragments and is completed mainly by simple methods of osteosynthesis.
Complex metal structures are rarely used in pediatric traumatology. Most often, a Kirschner wire is used for osteosynthesis, which, even when carried out transepiphyseally, does not have a significant effect on bone growth in length. The Bogdanov rod, CITO, Sokolov nails can damage the epiphyseal growth cartilage and therefore are used for osteosynthesis for diaphyseal fractures of large bones. 
For improperly fused and improperly fused bone fractures, false joints of post-traumatic etiology, compression-distraction devices of Ilizarov, Volkov-Oganesyan, Kalnberz, etc. are widely used.
The time frame for consolidation of fractures in healthy children is shorter than in adults. In weakened children suffering from rickets, hypovitaminosis, tuberculosis, as well as with open injuries, the periods of immobilization are extended, since the reparative processes in these cases are slowed down (Table 14.1).
With insufficient duration of fixation and early loading, secondary displacement of bone fragments and re-fracture are possible. Non-union fractures and pseudarthrosis in childhood are an exception and, with proper treatment, usually do not occur.
Delayed consolidation of the fracture area can be observed with insufficient contact between fragments, interposition of soft tissues, and repeated fractures at the same level.
After the onset of consolidation and removal of the plaster splint, functional and physiotherapeutic treatment is indicated mainly for children with intra- and periarticular fractures, especially when movement in the elbow joint is limited. Physical therapy should be moderate, gentle and painless.
Massage near the fracture site, especially with intra- and periarticular injuries, is contraindicated, since this procedure promotes the formation of excess callus and can lead to myositis ossificans and partial ossification of the joint capsule.
Children who have suffered injury near the epimetaphyseal zone require long-term follow-up (up to 1.5-2 years), since the injury does not exclude the possibility of damage to the growth zone, which can subsequently lead to limb deformity (post-traumatic deformity of the Madelung type, varus or valgus deviation of the limb axis, segment shortening, etc.).


Birth damage
Birth trauma includes injuries received during childbirth, as well as during the provision of manual assistance and revival of a child born in asphyxia.
More often, newborns experience fractures of the collarbone, fractures of the femur and humerus, and damage to the skull and brain. Fractures of the bones of the forearm and lower leg are extremely rare.
Clavicle fracture
In newborns, clavicle fracture occurs most often and is usually caused by pathological childbirth. Damage is possible during spontaneous childbirth in cephalic presentation, narrow pelvis, early rupture of water, etc. The fracture is usually localized in the middle third of the diaphysis and can be complete or incomplete (subperiosteal). In the area of the fracture there is slight swelling due to edema, hematoma, displacement of fragments and pathological mobility. In case of complete fractures, the child holds the arm in a forced position and does not move it, which gives rise to an erroneous diagnosis of Erb's palsy due to damage to the brachial plexus.
The most consistent sign of a clavicle fracture in newborns is crepitus of the fragments. With subperiosteal fractures, the diagnosis is often made at the end of the 1st week of the child’s life, when a large callus appears in the clavicle area.
Fractures of the humerus and femur in children
Such fractures are a consequence of obstetric care for foot or pelvic presentation of the fetus. Typical localization is in the middle third of the diaphysis of the tubular bone; along the plane, the fracture runs in a transverse or oblique direction. Traumatic epiphysiolysis of the proximal and distal ends of the humerus and femur are rare. This circumstance, as well as the fact that X-ray diagnostics are difficult due to the absence of ossification nuclei, often lead to untimely diagnosis of these injuries.
In diaphyseal fractures of the humerus and femur with complete displacement of bone fragments, pathological mobility at the level of the fracture, deformation, traumatic swelling and crepitus are noted. Any manipulation causes pain to the child. Fractures of the femur are characterized by a number of features: the leg is in the typical position of flexion in the knee and hip joints for a newborn and is brought to the abdomen due to physiological hypertension of the flexor muscles. Radiography clarifies the diagnosis.
There are several treatment options for newborns with diaphyseal fractures of the humerus and femur.
In case of a fracture of the humerus, the limb is immobilized for a period of 10-14 days. The arm is fixed with a plaster splint from the edge of the healthy scapula to the hand in the average physiological position or with a cardboard U-shaped splint in the position of shoulder abduction to 90°.
After immobilization, movement in the injured limb is restored in the near future without additional procedures and manipulations. For femur fractures in newborns, Schede traction is most effective. The immobilization period is the same. When monitoring the position of fragments, one should take into account the degree of permissible displacement of bone fragments (displacement in length up to 2-3 cm, in width - the full diameter of the bone, at an angle - no more than 25-30°), since self-correction and leveling will occur as they grow remaining offset; rotational displacements are not eliminated.
Traumatic epiphysiolysis in newborns has a typical picture and is more pronounced the more the fragments are displaced. Generic epiphysiolysis of the distal end of the humerus is often accompanied by paresis of the radial or median nerve.
X-ray diagnosis is practically impossible due to the lack of bone tissue in the area of the epiphyses, and only by the end of the 7-10th day on repeated X-rays can you see the callus and retrospectively decide on the nature of the former fracture.
The most typical mistake with this pathology is that a traumatic dislocation of the forearm bones is diagnosed and an attempt is made to reduce it, which, naturally, is doomed to failure. Treatment consists of one-stage closed reposition “by eye” followed by fixation in a light plaster splint in a mid-physiological position. At follow-up, a varus deviation of the forearm axis may be noted due to internal rotation of the humeral condyle that was not eliminated during treatment.
With epiphysiolysis of the proximal end of the femur, a differential diagnosis is made with congenital hip dislocation.
The injury is characterized by swelling, significant pain when moving, and possible bruising. Good results in the treatment of newborns with this injury are obtained by using a spacer splint. Immobilization period: 4 weeks With epiphysiolysis of the distal end of the femur in newborns, severe swelling and deformation in the knee joint are observed. During the examination, the characteristic “click” symptom is determined.
X-ray reveals a displacement of the ossification nucleus of the distal epiphysis of the femur, which facilitates diagnosis and allows, after reposition, to control the position of the fragments. The timing of clinical observation of children who have suffered a birth injury depends on the severity and location of the injury, but by the end of the first year of life it is possible, in principle, to resolve the issue of the outcome of the injury received at birth.
Clavicle fractures
Clavicle fractures are one of the most common bone injuries in childhood and account for about 15% of extremity bone fractures, second in frequency only to fractures of the forearm and humerus. In children, a clavicle fracture is caused by indirect trauma from a fall on an outstretched arm, on the shoulder or elbow joint. Less commonly, a clavicle fracture is caused by direct trauma—a direct blow to the collarbone. More than 30% of all clavicle fractures occur between the ages of 2 and 4 years.
With incomplete clavicle fractures, deformation and displacement are minimal.
The function of the arm is preserved, only its abduction above the level of the shoulder girdle is limited. Subjective complaints of pain are minor, so such fractures are sometimes not identified and the diagnosis is made only after 7-14 days, when a callus is detected in the form of a thickening on the collarbone. For fractures with complete displacement of fragments, the diagnosis is not difficult.
Clavicle fractures heal well, and function is fully restored with any treatment method, but the anatomical result may vary. Angular curvature and excess callus under the influence of growth disappear over time almost without a trace.
In most cases, a Deso-type bandage is sufficient to fix fragments for the entire period of treatment. For fully displaced fractures in older children, stronger fixation is required with the shoulder retracted and the external clavicle fragment elevated. This is achieved using an eight-shaped fixing bandage or a Kuzminsky-Karpenko crutch-plaster cast.
Surgical treatment is used extremely rarely and is indicated only when there is a threat of perforation by a skin fragment, trauma to the neurovascular bundle and interposition of soft tissues.
Scapula fractures
Scapula fractures are very rare in children. They arise as a result of direct trauma (falling on your back, blow, car injury, etc.). The most common fracture is the neck of the scapula, then the body and acromion. Fractures of the glenoid cavity, angle of the scapula, and coracoid process are exceptions. There is almost no displacement of fragments.A characteristic feature of scapula fractures is swelling, clearly demarcated, repeating the shape of the scapula (Comolli’s “triangular cushion” symptom).
This is caused by subfascial hemorrhage over the body of the scapula as a result of damage to the vessels supplying the scapula. Multiaxial radiography clarifies the diagnosis. Treatment consists of immobilization in a Deso-type bandage.
Rib fractures
Due to the high elasticity of the rib frame, rib fractures are not common in children. They are observed when the traumatic agent is of significant force (fall from a height, transport injury, etc.).The diagnosis is made on the basis of clinical manifestations and X-ray data. The child accurately indicates the location of the injury. Careless movements increase the pain.
Slight cyanotic skin, shortness of breath, and shallow breathing are noted due to fear of increased pain. Compression of the chest during the examination also causes pain to the child, so you should not resort to palpation if the patient reacts negatively.
Treatment of patients with uncomplicated rib fractures consists of intercostal novocaine blockade along the paravertebral line on the affected side, anesthesia of the fracture with a 1-2% novocaine solution and injection of a 1% pantopon solution in an age-specific dosage (0.1 ml per year of the child’s life, but not more than 1 ml ).
In case of severe symptoms of pleuropulmonary shock, it is advisable to perform a vagosympathetic blockade on the affected side according to Vishnevsky. Immobilization is not required, since tight bandaging of the chest limits the excursion of the lungs, which negatively affects the recovery period (complications such as pleurisy and pneumonia are possible).
With a direct and strong impact on the chest, multiple rib fractures may occur in combination with damage to internal organs.
Significant ruptures of lung tissue and damage to blood vessels are accompanied by severe bleeding into the pleural cavity, which leads to death.
Damage to the bronchi, causing tension pneumothorax, is also dangerous. The continued flow of air into the pleural cavity collapses the lung, displaces the mediastinum, and mediastinal emphysema develops. Bulau drainage or active aspiration are advisable for minor injuries to the lungs and bronchi. In case of bronchial ruptures, increasing hemopneumothorax, or open injury, urgent surgical intervention is indicated.
Sternum fractures
Sternal fractures in children are rare. They are possible with a direct blow to the sternum area. The most common site of injury is the junction of the manubrium of the sternum with the body.When fragments are displaced, sharp pain can cause pleuropulmonary shock. X-ray examination of the chest only in a strictly lateral projection allows us to identify the location of the fracture and the degree of displacement of the bone fragment.
Local anesthesia of the damaged area is effective, and in cases of pleuropulmonary shock - vagosympathetic blockade according to Vishnevsky. If there is a significant displacement of bone fragments, a closed reduction is performed or, according to indications, surgical intervention with fixation of the fragments with suture material.
Humerus fractures
Depending on the location, fractures of the humerus are distinguished in the area of the proximal metaepiphysis, diaphyseal fractures and in the area of the distal metaepiphysis.Typical types of damage to the proximal end of the humerus in children are fractures in the area of the surgical neck, osteoepiphysiolysis and epiphysiolysis, with typical displacement of the distal fragment outward with an angle open inward.
In fractures with displacement of bone fragments, the clinical picture is typical: the arm hangs along the body and the abduction of the limb is sharply limited; pain in the shoulder joint, swelling, tension in the deltoid muscle; with significant displacement (abduction fracture), a peripheral fragment is palpated in the axillary fossa. X-rays are performed in two (!) projections.
When indicated, reposition is usually performed in a hospital setting under general anesthesia and periodic X-ray monitoring. After reduction for abduction fractures, the arm is fixed in the average physiological position. In case of an adduction fracture with displacement of fragments, it is not always possible to compare bone fragments using conventional reposition, and therefore it is advisable to use the method developed by Whitman and M.V. Gromov.
During the reposition process, one of the assistants fixes the shoulder girdle, and the other carries out constant traction along the length of the limb, moving the arm upward as much as possible. At this time, the surgeon places the fragments in the correct position, pressing on their ends (be careful - the neurovascular bundle!). 
The arm is fixed with a plaster splint, which goes onto the body, in the position in which the correct position of the fragments was achieved (Fig. 14.3).
The duration of fixation in a plaster splint is 2 weeks (the time required for the formation of primary callus). On the 14-15th day, the thoracobrachial bandage is removed, the arm is transferred to the mid-physiological position and a plaster splint is again applied for 2 weeks (a total immobilization period of 28 days). Against the background of physical therapy and physiotherapy, movements in the shoulder joint are restored in the next 2-3 weeks.
In case of epiphysiolysis and osteoepiphysiolysis with significant damage to the growth zone in the long term, impaired bone growth in length can be caused. Dispensary observation is carried out for 1.5-2 years.
Humeral shaft fractures are uncommon in children.
The clinical picture is typical.
Fractures in the middle third of the humerus are dangerous due to possible damage to the radial nerve, which bends around the humerus at this level. Displacement of fragments can cause traumatic paresis or, in severe cases, disruption of the integrity of the nerve. In this regard, all manipulations for a fracture in the middle third of the diaphysis of the humerus must be performed with extreme caution.
The method of one-stage closed reduction followed by fixation in a plaster splint or the method of skeletal traction of the proximal metaphysis of the ulna is used, which gives the best result. If, during subsequent X-ray monitoring, secondary displacement of the fragments is detected, then it is eliminated by applying corrective rods. Pay attention to the correctness of the axis of the humerus, because displacement of bone fragments along the length of up to 2 cm is well compensated, while angular deformations during growth are not eliminated.
Fractures of the distal humerus are common in children.
They account for 64% of all humerus fractures.
For diagnosing injuries in the area of the distal metaepiphysis of the humerus, the most convenient is the classification proposed by G. A. Bairov in 1960 (Fig. 14.4).
Transcondylar and supracondylar fractures of the humerus are not uncommon in children.
The fracture plane in transcondylar injuries passes through the joint and is accompanied by rupture of the articular capsule and capsular-ligamentous apparatus (95% of all injuries). In supracondylar fractures, the fracture plane passes through the distal metaphysis of the humerus and does not penetrate the joint cavity (5%). The mechanism of injury is typical - a fall on an arm extended or bent at the elbow joint.
Displacement of the distal fragment of the humerus can be in three planes: anteriorly (with a flexion trans- or supracondylar fracture), posteriorly (with an extension fracture), outward - to the radial side or inward - to the ulnar side; rotation of the fragment around its axis is also noted. With significant displacement, disruption of innervation may occur as a result of injury to the ulnar, radial, transcondylar fractures of the humerus or median nerve. 
It is important to promptly identify peripheral circulatory disorders. The pulse in the radial and ulnar arteries may be absent for 4 reasons: due to post-traumatic spasm of arterial vessels, compression of the arterial vessel by a bone fragment or increasing edema and hematoma, and rupture of the neurovascular bundle (the most serious complication).
For trans- and supracondylar fractures of the humerus with displacement, conservative treatment is used in the vast majority of cases.
Closed reduction is performed under general anesthesia and periodic X-ray monitoring. The introduction of novocaine into the fracture area does not provide sufficient anesthesia and muscle relaxation, which makes it difficult to manipulate the fragments and keep them in the reduced position.
After a good comparison of bone fragments, monitoring the pulse is mandatory, since compression of the brachial artery by edematous soft tissue is possible. After reposition, a deep posterior plaster splint is applied in the position of the arm in which the bone fragments were fixed.
In case of significant swelling and failure of one-stage closed reduction, it is advisable to use the method of skeletal traction for the proximal metaphysis of the ulna with a load of 2 to 3 kg. If the fracture is unstable (more often observed with an oblique plane), you can use percutaneous fixation of bone fragments according to K. Papp (diafixation) or percutaneous osteosynthesis with crossed Kirschner wires according to the Judet technique.
If conservative treatment fails and there is unacceptable displacement of the fragments, open reduction may be necessary.
The operation is performed in extreme cases: with repeated unsuccessful attempts at closed reduction, with interposition of the neurovascular bundle between fragments with the threat of the formation of Volkmann's ischemic contracture, with open and improperly healing fractures.
Among the complications that are possible with this type of fracture, it should be noted myositis ossificans and ossification of the joint capsule. They are observed in children who undergo repeated closed reductions, accompanied by the destruction of granulations and primary callus. According to N.G. Damier, ossification of the joint capsule most often develops in children with a tendency to form keloid scars.
If internal rotation and inward displacement of the distal fragment of the humerus are not eliminated during treatment, they lead to varus deformity of the elbow joint.
When the forearm axis deviates by 15° in girls and 20° in boys, a corrective transcondylar wedge osteotomy of the humerus is indicated.
It is performed no earlier than 1-2 years after the injury using the Bairov-Ulrich method (Fig. 14.5). Preliminary calculation of the volume of proposed bone resection is important. X-rays of two elbow joints are taken in strictly symmetrical projections. 
The axis of the humerus and the axis of the forearm bones are drawn. Determine the value of the resulting angle a. The degree of physiological deviation of the forearm axis on the healthy arm is measured - angle /3, its value is added to the value of angle a and thus the angle of the proposed bone resection is determined.
The angle on the contourogram is drawn in the area of the distal metaphysis of the humerus at the level or slightly below the apex of the olecranon fossa.
The sides of the wedge should be as close to each other as possible. The stages of surgical intervention are presented in Fig. 14.6.
Fractures of the epicondyles of the humerus are typical injuries for childhood (most common in children from 8 to 14 years old).
They belong to apophyseolysis, since in most cases the fracture plane passes through the apophyseal cartilaginous zone. The most common avulsion of the medial epicondyle of the humerus occurs.
Its displacement is associated with tension on the medial collateral ligament and contraction of a large group of muscles attached to the epicondyle.
Often, separation of this epicondyle in children is combined with dislocation of the bones of the forearm in the elbow joint. When the capsular-ligamentous apparatus is ruptured, a displaced bone fragment can penetrate into the cavity of the elbow joint. In such a case, the apophysis is pinched in the humeroulnar joint; possible ulnar nerve paresis. The consequences of untimely diagnosis of a torn medial epicondyle embedded in the joint cavity can be severe: impaired articulation in the joint, stiffness, wasting of the muscles of the forearm and shoulder due to partial loss of arm function.
There are four ways to remove an osteochondral fragment from the joint cavity:
1) using a single-tooth hook (according to N. G. Damier);
2) reproducing the dislocation of the forearm bones with subsequent re-reduction (during manipulation, the fragment can be removed from the joint and reduced);
3) during surgery;
4) according to the method of V. A. Andrianov.
The method of closed extraction of the restrained medial epicondyle of the humerus from the cavity of the elbow joint according to Andrianov is as follows.
Under general anesthesia, the injured arm is held in an extended position and valgused at the elbow joint, which leads to widening of the joint space on the medial side. The hand is retracted to the radial side to stretch the forearm extensors.
With light rocking movements of the forearm and jerk-like pressure along the longitudinal axis of the limb, the medial epicondyle is pushed out of the joint, after which reposition is performed. If conservative reduction fails, open reduction with fixation of the medial epicondyle is indicated.
A fracture of the capitate eminence of the humerus (epiphysiolysis, osteoepiphysiolysis, epiphysis fracture) is an intra-articular fracture and most often occurs in children aged 4 to 10 years.
The damage is accompanied by rupture of the capsular-ligamentous apparatus, and the displacement of the bone fragment occurs outward and downward; Rotation of the capitate eminence up to 90° and even 180° is often observed. In the latter case, the bone fragment with its cartilaginous surface faces the fracture plane of the humerus. Such a significant rotation of a bone fragment depends, firstly, on the direction of the impact force and, secondly, on the traction of a large group of extensor muscles attached to the lateral epicondyle.
When treating children with a fracture of the capitate eminence of the humerus, one must strive for ideal adaptation of bone fragments.
Uncorrected displacement of the bone fragment disrupts articulation in the brachioradial joint, leading to the development of pseudarthrosis and contracture of the elbow joint.
In case of epiphysiolysis and osteoepiphysiolysis of the capitate eminence with slight displacement and rotation of the bone fragment up to 45-60°, an attempt is made at conservative reduction. During reposition (to open the joint space), the elbow joint is given a varus position, after which reduction is performed by applying pressure on the bone fragment from the bottom up and from the outside inwards.
If reposition is unsuccessful, and the remaining displacement threatens to cause permanent deformity and contracture, the need for surgical intervention arises. Open reduction is also indicated when the bone fragment is displaced and rotated by more than 60°, since an attempt at reduction in such cases is almost always unsuccessful. In addition, during unnecessary manipulations, existing damage to the capsular-ligamentous apparatus and adjacent muscles is aggravated, and the epiphysis and articular surfaces of the bones forming the elbow joint are unnecessarily injured.
Convenient surgical access to the elbow joint according to Kocher. After reposition, the bone fragments are fixed with two crossed Kirschner wires.
A good result is achieved using a compression device proposed by V. P. Kiselev and E. F. Samoilovich. Children who have suffered this injury are subject to clinical observation for 2 years, since damage to the growth zone with the formation of deformation in the later stages is possible.
Traumatology and orthopedics
Edited by corresponding member. RAMS
Yu. G. Shaposhnikova