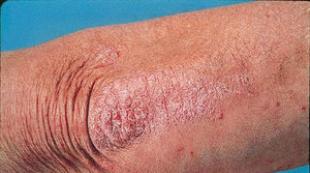
What is gastritis of the stomach? What is chronic gastritis type C
Gastritis is an inflammation of the mucous membrane (in some cases, even deeper layers) of the stomach wall. The disease leads to a decrease in the quality of food processing by gastric juice, due to which the entire functioning of the gastrointestinal tract is destabilized, and the body begins to experience a lack of substances even with a varied diet.
Symptoms include pain in the stomach on an empty stomach or after eating, nausea, vomiting, constipation or diarrhea, etc. Due to the many varieties of this disease, the term “gastritis” is collective and serves to designate inflammatory and dystrophic changes in the mucous membrane of this organ of various origins.
In the article we will consider: what kind of disease this is, what the causes and symptoms are, as well as how to treat gastritis in adults without consequences and follow a proper diet.
What is gastritis?
Gastritis (lat. gastritis) is an inflammation of the mucous layer of the stomach, leading to disruption of the functions of this organ. Gastritis is dangerous because if it is not treated correctly or if the mucous membranes of the stomach are damaged by concentrated acids, alkalis or chemicals, the disease can be fatal. In addition, gastritis can be a harbinger of oncological processes in the gastrointestinal tract (GIT).
The stomach is the most vulnerable part of the digestive system. At least three complex digestive processes occur in it: mechanical mixing of the food coma, chemical breakdown of food and absorption of nutrients. The inner wall of the stomach is most often damaged– the mucous membrane, where the production of two mutually exclusive components of digestion occurs - gastric juice and protective mucus.
Currently, gastritis can already be called the disease of the century. It affects both adults and children. And according to health statistics, in Russia about 50% of the population has gastritis in some form.
Reasons
Gastritis is manifested by inflammation and destruction of the gastric mucosa. The inflammatory reaction in the human body always develops in response to the action of damaging factors on healthy tissue. In the case of gastritis, it can be an infection, chemicals, high or low temperatures.

Thus, the main causes of this pathology are now placed as follows:
- the effect of bacteria and fungi on the walls of the stomach;
- eating disorders;
- alcohol abuse;
- taking medications;
- presence;
- chronic stress.
Internal causes of the disease include:
- hereditary predisposition to gastrointestinal diseases;
- presence of duodenal reflux;
- violation of the protective properties of cells at the immune level;
- hormonal imbalances;
- reflex transmission of pathogenesis from neighboring organs.
But the main cause of gastritis is a bacterium, which is found in 85% of registered cases.
Very often, the cause of gastritis is an incorrect diet:
- Hasty eating and poorly chewed food or dry food mechanically injure the mucous membrane
- Eating food that is too hot or too cold causes gastritis due to thermal damage to the stomach lining.
- Eating savory foods (mostly spicy and highly salted foods) irritates the stomach lining, similar to the effects of caustic chemicals.
Classification
Gastritis is classified according to several indicators - by type, by localization of the inflammatory process, by etiological factor, by endoscopic picture, by morphological changes in the gastric mucosa. All these indicators are very important for the diagnosis and choice of treatment for gastritis in adults.
Depending on the degree of damage and the duration of exposure to irritating factors, acute and chronic gastritis are distinguished.
Acute gastritis
Acute gastritis is understood as a single and rapid inflammation of the gastric mucosa caused by exposure to damaging factors of various etiologies (drugs, poisons, food contaminated with microorganisms, alcohol, etc.). With proper treatment, acute gastritis (depending on the form) lasts up to 5-7 days, but complete recovery of the stomach occurs much later.
Signs of acute inflammation of the mucous membrane appear suddenly and are caused by overeating, poor quality food, an allergic reaction to certain foods, and stress.
If factors that irritate the mucous membrane are not eliminated, inflammation passes into a chronic form.
Depending on the clinical manifestations and the nature of damage to the gastric mucosa, the following types of acute gastritis are considered:
- catarrhal - is the mildest form of the disease, in which only the very top layer of the gastric mucosa is affected. This type of gastritis occurs as a result of food poisoning or allergies to food or medications. The stomach can also suffer from severe emotional stress and overeating;
- fibrinous - with this form of gastritis, a protein is released at the site of inflammation - fibrin, which is contained in the blood plasma and has a fibrous structure. Externally, the site of such inflammation () is covered with a cloudy film of yellow-brown or gray color. Underneath it are numerous erosions of the mucous membrane, the formation of which can lead to an abscess, that is, phlegmonous gastritis. ;
- necrotic - not a very common form of gastritis; it occurs as a result of poisoning with chemicals. When, for example, acids enter the gastrointestinal tract, so-called coagulation necrosis is formed, if we are talking about salts - colliquation necrosis.;
- phlegmous - the most serious form of acute gastritis. May be a consequence of catarrhal gastritis. Accompanied by damage to all layers of the stomach. In the most severe cases it can be fatal. Requires immediate medical attention.
Chronic gastritis
Chronic gastritis is a long-term recurrent inflammation of the gastric mucosa, during which a number of dystrophic changes develop:
- increased infiltration,
- violation of the regenerative function of the glandular epithelium,
- proliferation of connective tissue.
Signs of chronic gastritis in adults are expressed in the following conditions:
- sweating after eating;
- losing weight;
- heartburn;
- pale skin;
- coated tongue.
According to etiology, chronic gastritis is divided into:
- Associated with the bacteria Helicobacter pylori.
- Autoimmune, caused by the formation of antibodies to stomach cells.
- Chemically mediated, that is, arising from long-term use of non-steroidal anti-inflammatory drugs (NSAIDs, or, in other words, NSAIDs) or the reflux of bile into the stomach.
- Idiopathic, that is, mediated by repeated exposure to the stomach of the same factor.
- Eosinophilic, allergic in nature.
- Granulomatous gastritis, which occurs along with granulomatous inflammation of other organs: Crohn's disease, tuberculosis, sarcoidosis, etc.
Also distinguished:
- Superficial gastritis
- Atrophic
- Reflux gastritis.
Depending on the secretory activity of the stomach, gastritis is distinguished:
- with high or normal acidity;
- with low or zero acidity.
It is quite possible to distinguish the symptoms of these conditions, but the final diagnosis is made on the basis of an analysis of gastric juice taken by intubation. In some cases, the pH of gastric juice is determined by indirect methods using urine tests.
Remember that only a doctor can determine the type, shape and course of gastritis. Under no circumstances take medications prescribed to your loved ones and friends - each individual form of gastritis requires an individual approach, and a drug that helped one person cope with gastritis can have a detrimental effect on the body of another.
Symptoms of gastritis in adults
How gastritis manifests itself in adults also depends on the individual characteristics of the patient’s body. Some patients patiently endure even the most severe pain, while others, at the first signs of damage to the inner lining of the stomach, experience many negative syndromes.

- weakness;
- vomiting;
- dizziness;
- epigastric pain;
- weight loss;
- cardiovascular disorders;
- drowsiness;
- irritability;
- lack of appetite;
- unpleasant taste;
- stool disorders.
The first signs of gastritis of the stomach
Gastritis has a variety of symptoms, but can occur without pronounced manifestations. The most characteristic sign:
- pain in the solar plexus area;
- aggravated after ingestion of certain types of food, liquids and medications, especially those with increased aggressiveness to the gastric mucosa;
- sometimes the pain intensifies between meals.
| Types of gastritis | Symptoms |
| Spicy | In acute gastritis, the following symptoms of gastric dyspepsia are observed:
|
| Chronic | Chronic inflammation of the stomach manifests itself as follows:
|
| With high acidity |
Patients with gastritis are bothered by pain in the epigastric region, night pain and hunger pain. |
| Low acidity |
|
The presence of at least one or more of the listed symptoms should force you to seek help from a gastroenterologist.
Complications
Gastritis of the stomach (with the exception of phlegmonous gastritis) does not belong to the group of dangerous diseases. However, gastritis gives rise to dangerous complications:
- internal bleeding: more typical for;
- hypovitaminosis;
- , sepsis: characteristic of purulent phlegmous gastritis;
- (anemia), vitamin B12 deficiency: develops due to inadequate absorption of vitamin B12 in the stomach. Anemia may develop for the same reason;
- : gastritis can become an impetus for the development of inflammation of the pancreas, especially in the presence of additional risk factors - drinking alcohol, taking medications, smoking;
- dehydration: with prolonged vomiting;
- : loss of appetite and metabolic disorders can lead to significant exhaustion of the body;
- gastric ulcer: in the absence or inadequate treatment, progression of damage to the stomach walls is possible;
- Stomach cancer: gastritis is a risk factor for the occurrence of gastric cancer.
Diagnostics
Diagnosis of any type of gastritis must necessarily include consultations with doctors such as a gastroenterologist and endoscopist. In order not just to suspect a pathological process, but to confirm that the assumptions are correct, the patient must be sent for a diagnostic examination.
When diagnosing gastritis, a specialist needs to establish the main cause of the pathology. Further therapy will largely depend on this.
The disease in adults is diagnosed using tests such as:
- gastroscopy - examination of the gastric mucosa with special equipment;
- biopsy;
- study of gastric juice in laboratory conditions;
- stool and blood analysis.
To identify Helicobacter pylori, a sample of a part of the mucous membrane removed during FGDS or blood is used - when examining it, it is determined whether it contains specific antibodies against the bacterium of interest.
Only the results of a comprehensive diagnosis allow a gastroenterologist to obtain a holistic picture, understand the causes of functional failure, and develop an individual treatment program.
Treatment of gastritis

In adults, treatment of gastritis is aimed primarily at eliminating factors that provoke the development or exacerbation of the disease (infection, unhealthy diet), stimulating restoration processes in the gastric mucosa and preventing new episodes of the disease (exacerbations).
How to treat gastritis of the stomach? It depends on the form of the disease. An important part of therapy is diet - without following certain rules of eating behavior, the medicinal effect will be much less effective.
Medications for gastritis:
- Antibiotics: amoxiclav, clarithromycin, metronidazole, furazolidone, amoxicillin. Medicines must be taken for at least 7 days, one tablet twice a day;
- Enveloping agents: gastal, phosphalugel, almagel - drugs that need to be taken three times daily for a month;
- Antisecretory drugs: omez, ranitidine, famotidine - take a tablet daily 20 minutes before meals. Medicines significantly reduce pain. The course of therapy is about a month;
- Antispasmodics: no-spa, platifilin, metacin - 3 tablets for severe pain;
- Cytoprotectors protect the gastric mucosa from the influence of hydrochloric acid - the duration of treatment is 20 days;
- Enzymatic preparations: pangrol, pancreatin, gastal, festal, mezim improve intestinal functionality. Take 1 tablet three times a day for a month;
- Hormonal agents improve the protective properties of the gastric mucosa;
- Antiemetic drugs: cerucal, metoclopramide - twice daily for a week.
You should not self-prescribe certain medications for yourself or your loved ones. This can lead to undesirable consequences and complications. A gastroenterologist knows how to cure gastritis.
After the onset of remission, you need to maintain regular eating up to 4-5 times a day, without long breaks. Do not overindulge in cold snacks, pizzas or hot dogs. It is advisable to completely avoid strong alcohol. Low-fat fermented milk products, boiled vegetables, lean meat and fish are shown.
Diet and treatment with folk remedies complement conservative therapy, which allows you to quickly achieve long-term remission.
The prognosis for all types of gastritis is favorable, but only with timely treatment, following a diet, and giving up bad habits. Do not forget that a long course of chronic gastritis can lead to the formation of adenocarcinoma and stomach cancer.
Diet
The diet for gastritis is different and depends on the form and stage of the disease. In the event of an attack, it is advisable to refuse food and drink for a day. This helps unload the stomach and intestines. If you are very thirsty, you can drink some still water at room temperature.
An exacerbation of the disease should be a signal to exclude from the diet:
- alcoholic drinks,
- coffee,
- marinades,
- seasonings,
- fried foods,
- sodas,
- conservation,
- semi-finished products,
- food from the fast food category,
- fatty foods,
- products that promote fermentation (grapes, black bread, milk),
- rich pastries.
If the disease is accompanied by increased acidity, a ban is imposed on:
- fried, fatty, spicy foods (digesting them requires an increased amount of hydrochloric acid),
- fresh fruits and vegetables,
- food with coarse fibers (lean meat, preferably veal, young poultry),
- Cereal porridges and soups should be high in mucus.
For gastritis with low acidity, the following dishes and ingredients should be included in the diet:
- Meat broths in the form of borscht soups or simply as a separate dish
- Bread made from wholemeal flour (with bran, rye).
- More fresh vegetables
- Various pickles that stimulate gastric secretion, increasing the pH of the stomach.
The appropriate temperature regime for consumed foods is also observed in the diet. It is important to consider that hot food causes damage to the inflamed mucous membrane, while cold food remains in the stomach for a longer time, due to which the production of hydrochloric acid increases. Again, foods fried in oil and fresh baked goods are excluded. All food, including soups, should be pureed and not hot.
How to treat gastritis with folk remedies
- Milk. This product helps to quickly reduce stomach acidity at home. In addition, drinking a glass of warm milk quickly eliminates the symptoms of heartburn.
- Flax. For therapy, you can only take cold-pressed oil, which contains the required amount of beneficial substances. The duration of treatment with flaxseed product is 12 weeks. During this period, the patient’s digestion will significantly improve and the harmful effects on the mucous membrane will decrease. To obtain the necessary therapeutic result, you need to take a teaspoon of oil before breakfast and after dinner. In this case, be sure to drink the product with a small amount of warm water, which ensures better absorption.
- Aloe juice has anti-inflammatory and powerful regenerative properties. Egg white is able to envelop the gastric mucosa, protecting against the aggression of hydrochloric acid. Mix these two ingredients 1:1 and drink a large spoon three times a day before meals.
- Gastritis in adults can be treated using thyme tincture. Take two tablespoons of herb and pour 500 ml. white wine, stand in the refrigerator for a week, then the resulting mixture must be boiled and strained. Take two teaspoons daily before each meal. This tincture helps patients with chronic gastritis to completely get rid of the disease.
- Mumiyo - a healing remedy from Altai which helps with gastritis. Mix a quarter gram of mumiyo with honey and milk, use the folk remedy daily on an empty stomach and before going to bed. It will be best if you add homemade milk to this cocktail; it interacts better with the other ingredients.
Prevention
As for preventive measures, they must be carried out on an ongoing basis. These include:
- giving up bad habits;
- maintaining proper, rational and balanced nutrition;
- compliance with the work and rest regime;
- physical activity;
- avoiding prolonged stressful situations and nervous overload
- undergo regular medical examination.
Preventive methods are not difficult to follow; they will help you maintain health, which is priceless.
Treatment of gastritis is a multifaceted process that includes diet, drug treatment, and strengthening the body's defenses. Gastritis should not be considered the norm, although it occurs in a huge part of the world's population, it must be treated.
This is all about gastritis of the stomach in adults (superficial, atrophic, reflux gastritis): symptoms, treatment features, medications. Don't get sick!
Material from Wikipedia - the free encyclopedia
| Gastritis | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ICD-10 |
To eliminate pain, take antispasmodics, anticholinergics, and antacids. It is recommended to take enterosorbents (smecta and others). For vomiting, prokinetics are prescribed. For acute toxicoinfectious gastritis - antibiotics (aminoglycosides, fluoroquinolones, biseptol and others). In severe acute gastritis, glucose solution, saline solution, and potassium preparations are administered parenterally to correct water and electrolyte disturbances. Chronic gastritisHouston classification chronic gastritis:
Other forms of gastritis also occur:
Etiology of chronic gastritisThe appearance and development of chronic gastritis is determined by the influence of many factors on the stomach tissue. The main external (exogenous) etiological factors contributing to the occurrence of chronic gastritis are: Internal (endogenous) factors contributing to the occurrence of chronic gastritis are: Helicobacter pyloriIn the second half of the 20th century, a previously unknown factor was identified, which today is considered one of the first places in the etiology of chronic gastritis. Helicobacter pylori is a spiral-shaped gram-negative bacterium that infects various areas of the stomach and duodenum. Many cases of gastric and duodenal ulcers, gastritis, duodenitis, and possibly some cases of gastric lymphoma and gastric cancer are etiologically associated with infection Helicobacter pylori. Successful experience with self-infection of one of the pioneers of the role Helicobacter pylori in the development of diseases of the stomach and duodenum - Barry Marshall and a group of volunteers served as convincing evidence of this theory. In 2005, Barry Marshall and his colleague Robin Warren were awarded the Nobel Prize in Medicine for their discovery. However, in the majority (up to 90%) of infected carriers Helicobacter pylori no symptoms of disease are detected. Not every chronic gastritis has a bacterial cause. ClassificationBy etiology Chronic gastritis is divided into three main forms:
In addition, there are also mixed - AB, A.C. and additional ( drug, alcoholic, etc.) types of chronic gastritis. Topographically distinguished:
Chronic gastritis and functional dyspepsiaChronic gastritis, manifested by persistent structural changes in the gastric mucosa, most often has no clinical manifestations. In Western countries, the diagnosis of “chronic gastritis” is rarely made recently; the doctor usually focuses on the symptoms of the disease and, on its basis, uses the term “functional dyspepsia”. In Russia, on the contrary, the diagnosis of “functional dyspepsia” is made very rarely; the diagnosis of “chronic gastritis” is used many times more often. In Japan, the country with the highest incidence of gastric cancer, the diagnoses of “chronic gastritis” and “functional dyspepsia” are combined, thereby indicating the presence or absence of changes in the gastric mucosa and/or corresponding clinical symptoms. Clinical manifestationsChronic gastritis is clinically manifested by both local and general disorders, which, as a rule, appear during periods of exacerbation:
DiagnosticsEstablishing a clinical diagnosis is based on determining the type of chronic gastritis, assessing the prevalence of morphological signs of the disease, the presence and severity of gastric dysfunction. Stages of diagnosing chronic gastritis:
Relief of exacerbation of chronic gastritisTreatment of relapse of chronic gastritis is carried out on an outpatient basis; the course of treatment, including diagnosis, is designed for 14 days. Among the medications for the treatment of chronic gastritis, proton pump inhibitors, H2-histamine receptor blockers, prokinetics, selective M-anticholinergics, and antacids are used. For some forms Helicobacter pylori- associated gastritis, eradication (destruction) is recommended Helicobacter pylori(see below)… Eradication Helicobacter pyloriAmong other forms of chronic gastritis, it predominates Helicobacter pylori- associated gastritis of the antrum of the stomach. For its treatment, the Maastricht III consensus meeting (2005) recommended a triple eradication regimen as first-line therapy, including one proton pump inhibitor and two antibacterial agents: clarithromycin and amoxicillin. If eradication fails, second-line therapy is proposed, including four drugs: a proton pump inhibitor, bismuth tripotassium dicitrate, metronidazole and tetracycline. At the same time, a number of experts believe that, due to possible problems that may arise as a result of taking antibiotics, eradication should be carried out Helicobacter pylori makes no sense, although there is a chance that it will help. However, other doctors believe that some forms of gastritis, in particular Helicobacter pylori- associated atrophic gastritis, requires mandatory eradication Helicobacter pylori. Reducing the acidity of gastric juiceIn the treatment of chronic gastritis, antisecretory drugs and enveloping agents are actively used. Medicines are used to suppress the secretion of hydrochloric acid in the stomach, which leads to a decrease in the acidity of gastric juice. The dose of antisecretory agents is selected individually. Vitamin preparations are used as additional therapy: vitamin U (methylmethionine sulfonium chloride) and B5 (pantothenic acid). Vitamin U (methylmethionine sulfonium chloride) is involved in the methylation reactions of biogenic amines and thereby reduces gastric secretion and provides an analgesic effect. Pantothenic acid (vitamin B5) promotes healing of the mucous membranes of the gastrointestinal tract and stimulates intestinal motility. Excess hydrochloric acid in the stomach often occurs precisely when there is a lack of pantothenic acid in the body. DietIn case of exacerbation of gastritis, a gentle diet is necessary. Patients with gastritis are contraindicated in chocolate, coffee, carbonated drinks, alcohol, canned food, concentrates and substitutes of any products, herbs, spices, as well as fast food products, dishes that provoke fermentation (milk, sour cream, grapes, black bread, etc.) , smoked, fatty and fried foods, pastry products. At the same time, food should be varied and rich in proteins and vitamins. After the end of the acute condition, nutrition should become complete, observing the stimulating principle during the period of remission in patients with low acidity. Small meals are recommended, 5-6 times a day. Write a review of the article "Gastritis"Notes
Literature
An excerpt characterizing GastritisThen she vividly imagined that moment when he had a stroke and was dragged out of the garden in the Bald Mountains by the arms and he muttered something with an impotent tongue, twitched his gray eyebrows and looked at her restlessly and timidly.“Even then he wanted to tell me what he told me on the day of his death,” she thought. “He always meant what he told me.” And so she remembered in all its details that night in Bald Mountains on the eve of the blow that happened to him, when Princess Marya, sensing trouble, remained with him against his will. She did not sleep and at night she tiptoed downstairs and, going up to the door to the flower shop where her father spent the night that night, listened to his voice. He said something to Tikhon in an exhausted, tired voice. He obviously wanted to talk. “And why didn’t he call me? Why didn’t he allow me to be here in Tikhon’s place? - Princess Marya thought then and now. “He will never tell anyone now everything that was in his soul.” This moment will never return for him and for me, when he would say everything he wanted to say, and I, and not Tikhon, would listen and understand him. Why didn’t I enter the room then? - she thought. “Maybe he would have told me then what he said on the day of his death.” Even then, in a conversation with Tikhon, he asked about me twice. He wanted to see me, but I stood here, outside the door. He was sad, it was hard to talk with Tikhon, who did not understand him. I remember how he spoke to him about Lisa, as if she were alive - he forgot that she died, and Tikhon reminded him that she was no longer there, and he shouted: “Fool.” It was hard for him. I heard from behind the door how he lay down on the bed, groaning, and shouted loudly: “My God! Why didn’t I get up then?” What would he do to me? What would I have to lose? And maybe then he would have been consoled, he would have said this word to me.” And Princess Marya said out loud the kind word that he said to her on the day of his death. “Darling! - Princess Marya repeated this word and began to sob with tears that relieved her soul. She now saw his face in front of her. And not the face that she had known since she could remember, and which she had always seen from afar; and that face is timid and weak, which on the last day, bending down to his mouth to hear what he said, she examined up close for the first time with all its wrinkles and details. “Darling,” she repeated. “What was he thinking when he said that word? What is he thinking now? - suddenly a question came to her, and in response to this she saw him in front of her with the same expression on his face that he had in the coffin, on his face tied with a white scarf. And the horror that gripped her when she touched him and became convinced that it was not only not him, but something mysterious and repulsive, gripped her now. She wanted to think about other things, wanted to pray, but could do nothing. She looked with large open eyes at the moonlight and shadows, every second she expected to see his dead face and felt that the silence that stood over the house and in the house shackled her. - Dunyasha! – she whispered. - Dunyasha! – she screamed in a wild voice and, breaking out of the silence, ran to the girls’ room, towards the nanny and girls running towards her. On August 17, Rostov and Ilyin, accompanied by Lavrushka, who had just returned from captivity, and the leading hussar, from their Yankovo camp, fifteen versts from Bogucharovo, went horseback riding - to try a new horse bought by Ilyin and to find out if there was any hay in the villages. - Well, honey? No, brother, my pink beauty, and their name is Dunyasha... - But, looking at Rostov’s face, Ilyin fell silent. He saw that his hero and commander was in a completely different way of thinking. Rostov, not wanting to impose his acquaintance on the princess, did not go to her, but remained in the village, waiting for her to leave. Having waited for Princess Marya's carriages to leave the house, Rostov sat on horseback and accompanied her on horseback to the path occupied by our troops, twelve miles from Bogucharov. In Yankov, at the inn, he said goodbye to her respectfully, allowing himself to kiss her hand for the first time. Having taken command of the armies, Kutuzov remembered Prince Andrei and sent him an order to come to the main apartment. | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Gastritis is a collective concept that unites inflammation of the gastric mucosa that differs in the reasons and method of development. As a result of such inflammation, metabolic processes are disrupted in the cells lining the stomach from the inside; they change structurally and are no longer able to perform their functions.
Ultimately, the cells can degenerate into cells of other organs (for example, into cells of the small intestine), leading to the formation of erosions, ulcers, and various polyps - which may be a reason to consult an oncologist.
Gastritis of the stomach is widespread in the world: about 63% of the world's population suffers from this disease, and most of them do not even know about their disease. Only 10-15% of them consult a doctor, which is explained by the fact that chronic gastritis, unlike an acute disease, often has mild symptoms and rarely bothers a person.
Causes of gastritis of the stomach
At the present stage, gastritis is considered as a disease that can occur either under the influence of one main factor or due to their combination. Main reasons:
- the presence of a specific bacterium Helicobacter pylori in the gastric mucosa (85% of chronic gastritis);
- autoimmune mechanisms (the body considers stomach cells as foreign and produces specific proteins for them - immunoglobulins);
- disruption of food transit through the gastrointestinal tract;
- food allergies;
- excessive use of drugs that damage the gastric mucosa;
- disturbance of the rhythm of nutrition, poor quality food, abuse of excessively hot or cold food, gastronomic features of food unusual for humans;
- smoking;
- alcohol abuse;
- occupational hazards (heavy industry, etc.);
- internal factors (chronic foci of infection - sinusitis, carious teeth, etc.; metabolic disorders (overweight and obesity, gout); diseases of the endocrine system).
Despite the huge number of causes of gastritis, they are all divided into:
- primary (when inflammation of the gastric mucosa is considered exclusively as a disease of this organ)
- secondary (inflammation occurs due to the painful state of other organs and systems, against the background of severe intoxication of the body).
Acute gastritis
Among them are acute and chronic gastritis. Acute gastritis is caused by the action of a strong irritant, for example, when consuming contaminated food, chemicals, or as a complication of metabolic disorders in the body, as well as during a serious illness. It most often has a pronounced clinical picture and vivid symptoms.
Chronic gastritis
Chronic gastritis is a characteristic inflammation of the gastric mucosa, which occurs due to a huge number of reasons and is characterized by a long and asymptomatic course. Doctors distinguish in this group autoimmune inflammation of the gastric mucosa, inflammation of the stomach under the influence of a special bacterium - Helicobacter pylori, as well as special forms of gastritis, for example, with renal failure.
Diagnosis of gastritis
Along with the enormous successes in diagnosing this disease, understanding the causes of its development, and advances in the creation of drugs, the results of treatment of gastritis (especially chronic gastritis) leave much to be desired.
The course of the disease is undulating, the symptoms are often erased, the disease is often advanced, adherence to treatment of patients without an exacerbation drops sharply, and adherence to diet and abandonment of bad habits when the attack of gastritis ends becomes burdensome.
Treatment of gastritis
Only a doctor should treat gastritis. You should not self-medicate: under the guise of relief, you can miss the development of formidable complications (stomach ulcers, obstruction, etc.). Acceptable treatment of gastritis at home, but under the systematic supervision of a doctor.
All treatment of gastritis is based on strict adherence to the rules of therapeutic nutrition (diet), a healthy lifestyle (quitting smoking and alcohol). It is doubtful to cure gastritis solely with diet (especially caused by H. pylori), but long-term remission is possible.
The diet has several basic principles:
- Meals should be nutritious, frequent, divided from 4 to 6 times a day. Dry food and overeating are excluded.
- Food should be gentle and not irritate the gastric mucosa (fatty meat and fish, dough products, vegetables and fruits high in fiber (peas, beans, etc.), chocolate, coffee, carbonated drinks, marinades, pickles, sour fruit juices are excluded ).
- The food should be dominated by vegetable fats and animal proteins, a reduced amount of carbohydrates (vegetable and milk soups, boiled low-fat fish and meat, scrambled eggs, noodles and crackers made from white flour, low-fat cottage cheese, vegetable purees, milk, weak tea, vinaigrette with vegetable oil).
Drug treatment of gastritis
In the process of such treatment, several main goals are achieved.
First, reducing the acidity of gastric juice, which in medical practice is achieved by prescribing 3 groups of drugs:
- Proton pump inhibitors (rabeprazole, omeprazole, etc.)
- Histamine blockers (famotidine, etc.)
- Antacids (Almagel, Hefal, etc.)
Second, normalization of motility in all parts of the gastrointestinal tract is achieved by taking prokinetics (Motilium, Cerucal).
Third, protect the cells of the gastric mucosa. For this purpose, mucus production enhancers (biogastron, etc.) and recovery stimulants (sea buckthorn oil, solcoseryl, etc.) are widely used. Modern medicine - synthetic analogues of prostaglandins (for example, misoprostol) - is effective, but too expensive.
Fourth, removal of H. pylori, if such a bacterium is present in the stomach.
For this, treatment regimens are prescribed, consisting of 2 antibiotics, a proton pump inhibitor, and a bismuth drug.
Symptoms of gastritis
There are a large number of symptoms by which a person may suspect gastritis. Based on their combination, one can with a certain degree of confidence assume the acute or chronic nature of inflammation in the gastric mucosa.
Diagnosis of acute gastritis is not very difficult.
Firstly, a person can quite accurately indicate what causes a sharp deterioration in health (poor food, alcohol abuse, etc.).
Secondly, the symptoms of gastritis, which occurs in acute form, can be divided into two large groups:
- signs characteristic of inflammation of the stomach itself
- and signs of general intoxication (malaise) of the body.
The first group includes:
- sharp, cutting pain in the upper third of the abdomen or, conversely, unpleasant heaviness in the abdomen, alleviated after taking milk, a small amount of food or water, soda, taking antacids (Gefal, Almagel, etc.).
- Often, the first signs of acute gastritis begin with painful nausea, which can be replaced by repeated vomiting, which brings relief. It most often has an unpleasant sour-bile taste that remains in the mouth for a long time.
- often this is accompanied by heartburn- an unpleasant sensation of heat, strong warmth behind the sternum, which can intensify when lying on your side, but goes away somewhat while walking or standing.
Common symptoms that occur due to inflammation of the gastric mucosa are general weakness, lethargy, loss of mood and appetite, and a slight rise in body temperature.
Signs of gastritis
The signs of chronic gastritis are numerous, but, as a rule, they are erased and slightly expressed (in rare cases - chronic gastritis proceeds with a violent picture of the disease). Over the course of months, years or even decades, this disease may simply not bother you.
The most common symptoms with which “gastritis of the stomach” begins:
- an uncomfortable feeling of heaviness, pressure or fullness in the upper third of the abdomen, which is long-lasting and permanent;
- recurring heartburn;
- nausea ;
- unexpressed, aching without clear localization stomach pain, which occurs after errors in eating (consumption of spicy, fatty, overcooked foods or alcohol; when eating quickly (hurriedly);
- belching air, eaten food (after which the pain decreases);
- decreased appetite;
- metallic taste in the mouth;
- bowel dysfunction;
- frequency of symptoms: autumn, spring - but with autoimmune gastritis, the symptoms are constantly expressed.
In cases where gastritis is complicated by the development of erosions or ulcers, characteristic cutting or sharp stabbing pains are added to this. In this case, you must immediately consult a doctor.
In advanced cases, when the gastric mucosa can no longer perform its functions (enzyme production, food digestion and partial absorption of nutrients), the general symptoms of “stomach gastritis” come to the fore: weakness, pallor, lack of satiety after eating, weight loss, fragility nails and hair (signs of insufficient digestion). At the same time, bleeding gums, bumps in the corners of the mouth may indicate vitamin deficiency, which develops with a long course of the disease. Often, chronic gastritis (especially atrophic) can cause the development of anemia.
It is worth noting that the above signs of gastritis are most clearly presented during an exacerbation, while during the period of remission (outside of an exacerbation) their expression is unclear and blurred.
Diet for gastritis
Therapeutic nutrition for diseases of the digestive system is of paramount importance. Treatment of gastritis solely with diet cannot cure the disease, but significantly alleviates the course of the disease and eliminates the symptoms. The main provisions of such nutrition are formulated as follows.
Firstly, nutrition for gastritis should be varied, complete in energy value and the composition of proteins, fats, and carbohydrates. Foods that are not typical for the region in which the patient lives are excluded from the diet. A minimum content of salt and spices (especially hot ones) is achieved in food. Dietary recipes include dishes prepared according to the principle of mechanical, chemical and thermal sparing (these are ground and mashed dishes, neither hot nor cold by the time of serving).
Secondly, nutrition for gastritis of the stomach must be carried out four to six times a day, regularly, at the same time. The evening meal should take place at least 2-3 hours before going to bed.
Thirdly, it is advisable to exclude eating on the go, overeating, and dry eating. The menu for gastritis should consist of 3, at least 2 dishes. Eating hot food at least 2 times a day. First - at least 1 time per day.
Fourthly, when planning your diet for the week, it is recommended to increase the proportion of vegetable fats in the menu by 15-20%, and animal proteins by 15%. It is believed that this combination of proteins and fats has pronounced restorative properties for the cells of the gastric mucosa. It is also worth sharply limiting, by about half, animal fats and carbohydrates.
Menu for gastritis
The diet for gastritis consists of avoiding cooking dishes that increase the secretion of gastric juice (mushroom, fish and meat soups and broths).
Vegetables and fruits with a high fiber content (legumes, turnips) are contraindicated for this disease.
In recipes, be careful to include a small amount of low-fat cottage cheese and non-acidic cheese.
You should be careful with fatty meats and fish.
Flour products, buns and pies are replaced with crackers.
Unripe fruits and berries with rough peels, various juices, strong tea and coffee, chocolate, carbonated water, canned food, pickles and spicy seasonings, smoked marinades are strictly contraindicated for gastritis.
What is possible?
Proper nutrition consists of the following:
- vegetable soups, cereals, milk soups
- Boiled meat and fish of low-fat varieties
- steamed meat and fish
- boiled porridge
- durum wheat noodles
- vegetable puree, mashed potatoes
- non-sour cottage cheese
- milk
- dairy products such as yoghurts and fermented baked milk
- alkaline mineral waters without gas
- non-acidic juices with pulp from fruits and berries
- weak tea
Dietary nutrition for gastritis with low acidity has some features. Firstly, instead of slimy vegetable soups, which are indicated for high acidity, it is recommended to drink a small amount of black currant juice 1-2 times a day. Secondly, the diet for patients with gastritis in this case includes kefir and cottage cheese.
It is worth noting that during the non-exacerbation period, an important role is played not only by the quality of food preparation, but also by sufficient provision of the body with vitamins and minerals. At this stage, you can take multivitamins or baby food purees.
Gastritis in children
In children, the development of inflammation of the gastric mucosa occurs for the same reasons as in adults. There are acute and chronic, primary and secondary gastritis.
The most common age of development of the disease is 5-7 and 9-13 years. Before puberty, the frequency of occurrence in boys and girls is approximately the same, after which girls suffer more often.
Acute gastritis most often develops against the background of overeating, eating poor quality food, or poisoning with spoiled foods. Often, the cause of gastritis is food with a high content of food allergens (large amounts of spices, exotic varieties of fish and meat, fruits).
Separately, gastritis is distinguished, which develops while taking certain medications that adversely affect the gastric mucosa (antipyretics, some antibiotics).
Gastritis can also develop against the background of a poorly tolerated childhood infection ( measles , rubella , flu etc.).
Symptoms of gastritis in children
You should know that in young children, the fundamental symptoms of gastritis may not be expressed, masking as nonspecific signs of general malaise and intoxication.
Most often, at this age, parents are concerned about the development of nausea and vomiting in their child. In this state, children most often do not behave as actively as usual. They are lethargic, refuse to eat, or stop playing. You may notice increased production of saliva or, conversely, young children complain of constant dry mouth and often ask for a drink.
Parents may be alarmed by the child's low body temperature and frequent vomit, rumbling in the stomach, diarrhea.
In case of poisoning or severe gastritis, the child’s temperature may rise sharply, the pulse may increase, and consciousness may become confused. In such cases, the abdomen is swollen, there are no peristaltic sounds, or, conversely, rumbling and transfusion in the abdomen are clearly audible. In such cases, it is necessary to immediately take the child to the doctor to exclude an acute surgical disease (appendicitis, acute gastric ulcer and/or its complications).
Determining gastritis in older children does not cause great difficulties - the signs of gastritis are similar to those in adults.
Treatment of gastritis in children
Treatment of the disease in children has a number of features compared to adults.
The main task is to eliminate the cause of gastritis. They give smecta and activated carbon according to the age norm.
During the first 2 days, strict bed rest is indicated. The stomach is washed with a weak solution of soda and mineral water until the water is clear. The child is given frequent warm drinks over the next 12 hours.
In case of severe pain, you can give the child antispasmodics (for example, no-spa), a small amount of antacids (Almagel).
The diet for gastritis in children is as follows. After 1-2 days of fasting, you can give kefir, low-fat broth, jelly, porridge cooked in water - this diet is followed for the first 3-4 days. On days 5-7, it is allowed to give the child low-fat cottage cheese, white bread croutons, and soft-boiled eggs.
If the leading role of microorganisms in the development of gastritis (poisoning) is established, the leading role is occupied by the prescription of antibiotics. If worms are detected, use appropriate medications (acaris, etc.).
The tactics for managing chronic gastritis in children are similar to those in adults (see “Chronic gastritis”).
Acute gastritis
Acute gastritis is an inflammation of the gastric mucosa that occurs against the background of short-term exposure to strong irritants (acids, alkalis, various infections, etc.).
Most often, this condition develops suddenly, against the background of complete health. In such cases, a person can remember the moment the first symptoms appeared for up to hours. Often he can independently associate his condition with a specific cause (eating errors, drinking alcohol, taking acid or alkali, etc.).
Acute gastritis in most cases has a severe course and is poorly tolerated by people.
It is necessary to distinguish between acute gastritis and exacerbation of gastritis, which has already entered the chronic stage. The symptoms of the two conditions are similar, but treatment tactics in such cases are somewhat different.
Reasons for the development of gastritis:
- gastronomic excesses and errors in food (alcohol, excessively salty and peppery foods, smoked foods, marinades, etc.);
- intentional or accidental use of aggressive substances (acids, alkalis, etc.);
- overdose or prolonged and systematic use of certain medications (steroid hormones, aspirin, etc.);
- secondary gastritis developing against the background of other diseases, injuries ( myocardial infarction, kidney failure, burn disease, etc.);
- intestinal infections (shigellosis, staphylococcal infection, etc.);
- Helicobarcter gastritis;
- psycho-emotional overload (stress ulcers and erosions).
Symptoms of acute gastritis
As a rule, the disease begins suddenly. There is heaviness in the stomach, nausea followed by vomiting, which brings relief. The second option for the onset of the disease may be a severe pain syndrome, starting with sharp, cutting pain in the upper and/or middle third of the abdomen. Joins vomit eaten food. The pain is excruciating, constant, weakens or temporarily disappears after taking a small amount of milk, antacids (Almagel, Hefal, etc.).
There is a sharp deterioration in general health: no appetite, mood disappears, weakness appears, lethargy, malaise.
Along with the pain, a slight fever appears. If gastritis is caused by intestinal microorganisms, the temperature may precede abdominal discomfort and reach significant numbers.
After a while it appears diarrhea, which may be accompanied by ongoing vomiting.
When consuming chemically active substances (acids, alkalis, etc.), the symptoms of inflammation of the gastric mucosa are accompanied by signs of a burn of the esophagus (severe heartburn, increased salivation), oral mucosa (loss of taste, drooling).
Treatment of acute gastritis
You should firmly know that acute gastritis is a disease that requires the participation of a doctor. Self-medication and untimely contact with a doctor can cause death, because... Under the mask of acute gastritis, a large number of emergency surgical situations can be hidden: from appendicitis to perforation of a stomach ulcer into the abdominal cavity! After providing first aid, contact a specialist.
Treatment of acute gastritis begins with removing the cause of the disease: gastric lavage with a sufficiently large amount of water or mineral water, taking adsorbents (polyphepam, activated carbon, etc.) are indicated.
If gastritis has developed due to the intake of aggressive liquids - acids, rinsing is carried out with a weak solution of boric acid or soda. If inflammation develops under the influence of alkalis, add citric acid to the solution. Then add a small amount of sea buckthorn oil or Vaseline to protect the mucous membrane from the irritant.
The patient is given plenty of warm, frequent drinks. In case of severe vomiting or diarrhea, a person needs to drink (even with force!) up to 8 liters of mineral water or special solutions containing electrolytes (Regidron, etc.).
The diet for acute gastritis consists of complete fasting for the first 1-2 days. Afterwards, with great caution, you can eat pureed rice or semolina porridges cooked in water. Weak tea is allowed.
After 3-4 days from the onset of the disease, add a small amount of low-fat (most often chicken) broth with white bread croutons, kefir, steamed omelet or soft-boiled eggs.
Starting from days 5-7, the diet is expanded, you can eat boiled meat, buckwheat porridge - “smear”, white bread (but more acceptable - crackers), low-fat cottage cheese.
By the end of the first week, you can eat everything, but with great caution. Salty, smoked, pepper and marinades should be avoided. Carbonated water, chocolate, milk, sour cream, mayonnaise are prohibited for the next 2-3 weeks. The diet after acute gastritis is not much different from that for chronic gastritis.
Chronic gastritis
This is a disease that is characterized by prolonged inflammation of the gastric mucosa with characteristic changes.
It should be noted that this diagnosis can only be made absolutely accurately using a microscope. When conducting a special study - fibrogastroduodenoscopy - an endoscopist takes several pieces of the gastric mucosa. When examining pieces of tissue under a microscope, this diagnosis is confirmed or refuted, the degree of atrophy, dysplasia, metaplasia of stomach cells is determined, and infection with a specific bacterium - Helicobacter pylori - is determined.
Chronic gastritis is widespread among the world's population. According to statistics, more than half of all people suffer from this disease.
Chronic inflammation of the gastric mucosa for reasons of development is divided into four main types:
- type “A” (gastritis of the body of the stomach) is based on autoimmune mechanisms, as a result of which antibodies are produced to the cells of the stomach.
- type “B” (antral gastritis) - it is believed that it is caused by the specific bacterium H. pylori, discovered at the beginning of the 21st century.
- type “C” develops under the influence of various chemicals, alcohol, and some medications.
- the next type develops as a result of prolonged exposure to contents from the duodenum (most often bile), which is thrown into the stomach as a result of insufficiency of the sphincter muscle sphincter.
- Some researchers classify as a separate group inflammation of the gastric mucosa that occurs after operations on this organ - post-resection gastritis.
In cases where the duodenal mucosa is involved in inflammation, the disease is called “gastroduodenitis.”
Another classification identifies two main types of gastritis, depending on which the doctor uses different treatment tactics.
This is chronic gastritis with and without the development of atrophy.
Atrophy is a condition in which the cells of the stomach change, lose the structure characteristic of this organ and cannot fully realize their functions (secretion of mucus, enzymes, hydrochloric acid). Such cells are no longer capable of absorbing useful substances (proteins, vitamins, small amounts of carbohydrates and fats broken down into amino acids).
Chronic gastritis is also distinguished with increased or decreased acidity of gastric juice (see “Gastritis with low acidity”, “Gastritis with high acidity”).
Symptoms of chronic gastritis.
The disease can have a clear picture only at the beginning of its development. In most cases, chronic gastritis develops gradually, unnoticed by a person. The signs of such gastritis are most often blurred, not clearly expressed - and a person may not even be aware of the presence of the disease for a long time.
Depending on the type of gastritis and the pH level of gastric juice, all symptoms can be divided into two large groups:
1. signs more characteristic of chronic gastritis with low acidity and atrophic gastritis (unexpressed dull, aching pain in the upper third of the abdomen; a feeling of discomfort, heaviness, bloating in the abdomen after eating; increased gas formation, rumbling in the abdomen and periodic loose stools or constipation, unpleasant bad breath).
2. signs more characteristic of chronic gastritis with increased acidity of gastric juice, erosive or superficial gastritis (severe “hungry” abdominal pain on an empty stomach or at night; sour belching; heartburn; pain in the upper third of the abdomen after a diet violation).
Treatment of chronic gastritis
The treatment tactics for this disease are complex: simultaneous prescription of medications and nutritional therapy (diet).
All medications used in treatment can be divided into four large groups:
- drugs that reduce gastric acidity
- drugs that normalize digestive processes in the gastrointestinal tract
- stimulators of gastric cell regeneration
- antibacterial drugs to eradicate (remove) H. pylori infection
More detailed treatment is discussed in the section “Treatment of gastritis”.
Nutrition for chronic gastritis is based on the principles of protecting (sparing) the gastric mucosa. This is achieved by steaming dishes, pureed soups and cereals, and limited consumption of fresh juices and fruits high in fiber. A diet for chronic gastritis requires frequent divided meals, preferably at the same time, a balance of proteins, fats and carbohydrates. Products must contain sufficient amounts of minerals and vitamins (see “Diet for gastritis”).
Atrophic gastritis
The most common form of chronic gastritis. It is found in approximately 70-75% of all those suffering from chronic inflammation of the gastric mucosa. Most often, elderly people or those who have been ill for a long time suffer.
Atrophy is a condition in which the cells of the stomach change, lose the structure characteristic of this organ and can no longer fully realize their functions (secretion of mucus, enzymes, hydrochloric acid). Such cells are not capable of absorbing useful substances (proteins, vitamins, small amounts of carbohydrates and fats broken down into amino acids).
The diagnosis of chronic gastritis with atrophic changes is made according to a typical clinical picture, very similar to that of gastritis with low acidity of gastric juice, and is confirmed by microscopic examination of pieces of mucous membrane taken during fibrogastroduodenoscopy.
Symptoms of atrophic gastritis
As already mentioned, this form of gastritis can be suspected by typical symptoms, also characteristic of gastritis with low acidity. In addition, low acidity is a constant companion to such inflammation of the gastric mucosa.
Most often, atrophic gastritis of the stomach can be suspected by symptoms of impaired digestion, passage of food through the gastrointestinal tract, and metabolic disorders.
It is characterized by a feeling of heaviness in the stomach after eating, discomfort in the upper third of the abdomen that is constant or worsens after errors in the diet, etc. (for more details, see “”).
Such people experience chronic anemia (decreased hemoglobin levels in the blood), poor skin and hair condition (dull, brittle hair, oily or dry skin, flaking). We are concerned about weakness and malaise, which can haunt a person for many months and years and cause him to turn to a huge number of specialists. This is often accompanied by weight loss while maintaining a normal diet.
Against the background of developing hypovitaminosis, pustular skin lesions and seizures in the corners of the lips appear. Immunity decreases, leading to frequent viral diseases.
Treatment of atrophic gastritis
The treatment tactics for such gastritis are the same as for gastritis with low acidity (see “Gastritis with low acidity”).
Enzyme preparations are prescribed to restore digestion. In advanced cases, the use of gastric juice is indicated.
Drugs that stimulate the restoration of stomach cells (solcoseryl, sea buckthorn oil, etc.) are actively prescribed.
Diet is of great importance for patients with atrophic gastritis. Its basic principles do not differ from nutritional therapy for other types of gastritis. The only exception is the consumption of slimy soups and cereals, which are replaced with fresh juice and low-fat broth.
Treatment of atrophic gastritis with folk remedies has no independent meaning and is used only in complex therapy. Propolis tinctures, honey, chamomile and sage decoctions are used (for more details, see “Treatment of Gastritis”).
It should be remembered that atrophic gastritis can become the basis for the development of precancerous conditions - and thus requires systematic medical supervision.
Gastritis with high acidity
This is an inflammation of the gastric mucosa, which is accompanied by an increase in the acidity of gastric juice.
This type of gastritis most often occurs in young people and has several causes for its development. Based on them, four forms of gastritis with high acidity are distinguished.
The development of gastritis type “A” (“fundal gastritis”) is based on autoimmune mechanisms, as a result of which antibodies are produced to the cells of the stomach.
Gastritis type "B" (antral gastritis) - is believed to be caused by a specific bacterium, H. pylori.
Type “C” gastritis develops under the influence of various chemicals, alcohol, and some medications. And reflux gastritis, which develops due to the reflux of the contents of the small intestine back into the stomach.
Symptoms and signs of gastritis with high acidity
It is believed that gastritis with high acidity is characterized by a wave-like course with periods of exacerbations (most often in autumn and spring) and remissions.
At the beginning, the pain is constant, aching, moderate, sometimes manifested in the form of pressure, heaviness in the pit of the stomach. Most often they are provoked by errors in food (overcooked, fatty and smoked foods).
A rare but characteristic symptom is “late” hunger pain, which occurs 6-7 hours after eating. The pain is so severe that it is similar to that of a stomach ulcer.
Often, problems with stool (constipation) appear.
Signs of gastritis with high acidity outside of exacerbation are most often not expressed. May be a minor concern heartburn , belching air or recently eaten food.
Treatment of gastritis with high acidity.
When treating gastritis of this type, several goals are simultaneously pursued.
Firstly, reduction of total acidity (this is achieved by prescribing special drugs from the group of proton pump inhibitors (PPIs) - omeprazole, rabeprazole, etc., histamine receptor blockers - famotidine, etc.; the use of antacids (Almagel, etc.).
Secondly, To normalize digestive processes, enzymatic preparations (festal, mezim, etc.) are prescribed.
Thirdly, if gastritis is caused by H. pylori, then antibiotic therapy comes first. Currently, there are 2 main treatment regimens: 3-component or 4-component. The joint prescription of 2 antibiotics and an acid-reducing drug (PPI) is three mandatory components. Additional administration of bismuth preparations is typical for a 4-component regimen.
It must be remembered that the basis of any treatment for gastritis is diet and avoidance of alcohol and smoking. The food excludes dishes that stimulate secretion in the stomach (marinades, smoked meats, pickles, hot seasonings). Meals are frequent, split meals (from 4 to 6 times a day), preferably at the same time, gentle, steamed or with a minimum amount of fat and oil. Various vegetable or fish side dishes, lean meats (chicken, veal) are welcome; a special place is occupied by the consumption of soups, which should be included in the diet at least 2 times a day. The use of enveloping substances (flax seed decoction, white clay, antacids) is also recommended both during an exacerbation and outside of it.
During an exacerbation, treatment consists of complete cessation of smoking, alcohol, and fasting for 1-2 days. Antacids (Almagel, Hefal, etc.) and proton pump inhibitors are taken. It must be remembered that the symptoms of gastritis with high acidity during an exacerbation are similar to the signs of an acute ulcer of the stomach or small intestine. You must immediately stop self-medication and consult a doctor.
Gastritis with low acidity
This is an inflammation of the gastric mucosa, which is accompanied by a decrease in the acidity of gastric juice.
Such gastritis occurs in 20-25% of newly diagnosed cases of chronic gastritis, and reaches values of up to 60% in advanced forms of this disease. This is explained by the fact that during the transition of acute gastritis to chronic gastritis, in most cases, high acidity levels of the stomach contents are observed, but over time, the acidity values decrease.
Chronic gastritis with low acidity is typical for older people who have been suffering from inflammation of the gastric mucosa for a long time.
The reasons for the development of the disease are the same as for chronic gastritis with high acidity (there are 4 types: “A”; “B”; developing under the influence of various chemicals; reflux gastritis).
Symptoms of gastritis with low acidity
The release of hydrochloric acid by stomach cells is a necessary condition for the activation of a large number of enzymes of the digestive system. For example, pepsin, the main enzyme of gastric juice, which breaks down proteins in the lumen of the stomach, passes from an inactive form (pepsinogen) to an active one (pepsin itself) only at low pH. In addition, the acidic contents of the stomach are a direct regulator of the movement of the bolus of food into the lower gastrointestinal tract.
Thus, for gastritis with low acidity, symptoms associated with the quality of food digestion come to the fore, and very rarely, severe pain.
Patients suffering from this type of gastritis complain of a feeling of heaviness, fullness, and distension in the upper and middle third of the abdomen, especially after eating.
Treatment of gastritis with reduced activity.
The treatment achieves several goals.
- Firstly, restoring the activity of enzymes in the digestive system.
- Secondly, achieving proper regular functioning of all parts of the digestive tract.
- Thirdly, normalization of digestion.
- Fourthly, if H. pylori is detected, antibiotics are prescribed.
Due to the symptoms not being as pronounced as with gastritis with high acidity, the main place is not medicinal treatment, but adherence to therapeutic nutrition (diet) and a healthy lifestyle (quitting smoking, drinking alcohol).
The diet corresponds to that for gastritis with high acidity, with minor exceptions: slimy vegetable soups and cereals are removed from the menu and a small amount of fermented milk products (kefir, non-sour cheese), fresh berry juice with pulp is added (see “Diet for Gastritis”) .
Enzymes (Pancreatin, Creon, Mezim, etc.) are prescribed to compensate for their insufficient activity, especially when the acidity of gastric juice is extremely low.
To regulate the functioning of the entire gastrointestinal tract, drugs that regulate digestion are prescribed - metoclopramide and domperidone (Motilium, Cerucal, etc.).
Antral gastritis
In modern classifications, this type of gastritis is called “type “B” gastritis. This gastritis is diagnosed based on the results of a biopsy and examination of stomach tissue under a microscope. The basis for its occurrence is considered to be the specific bacterium Helicobacter pylori.
Gastritis got its name because it is characterized by inflammatory changes in the part of the stomach called the “antrum”. Let us recall that the stomach is conventionally divided into 3 regions: the cardia (the uppermost part), the body (the middle part) and the antrum (the lower region at the junction of the stomach and the duodenum). It is in the antrum that the contents of the stomach are gradually alkalized and prepared for passage into the intestine.
Antral gastritis is especially studied because in 100% of cases of acute or chronic ulcers of the duodenum or stomach it is detected by microscopic examination. It is believed that antral gastritis is a direct factor in the formation of ulcers.
Three quarters of all antral gastritis occurs with increased acidity of gastric juice, the rest with normal acidity. A peculiarity of the symptoms of such inflammation of the gastric mucosa is that even at low pH values, a person most often does not feel the disease. He may only periodically be bothered by minor pain in the upper third of the abdomen and slight belching.
Treatment of antral gastritis
Treatment of gastritis with a predominant lesion of the antrum is carried out according to the general scheme (drugs that increase the pH of gastric juice, prokinetics, stimulators of gastric cell restoration, regulators of digestive activity and enzymes) (in more detail - “Treatment of gastritis”).
A special feature is that the treatment regimen includes aggressive antibacterial therapy aimed at removing Helicobacter pylori from the gastric mucosa. A 3-component combination of drugs (a proton pump inhibitor and two antibiotics) or a 4-component combination of drugs is prescribed (in this case, bismuth drugs are added). The course of therapy lasts from 10 to 14 days. Control fibrogastroduodenoscopy is performed 2, 4 and 8 weeks after treatment. Even after a positive result from the therapy, it is necessary to be systematically observed by the attending physician for early detection of relapse of the disease.
It is worth noting that the wording “superficial antral gastritis” implies inflammation of the gastric mucosa with a predominant localization in the antrum, which, according to the development mechanisms and characteristic microscopic picture, is the same as type B gastritis.
Erosive gastritis
Erosive gastritis is one of the most common types of gastritis, which is characterized by superficial damage to the gastric mucosa in the form of characteristic defects - erosions.
Erosion of the stomach or duodenum is currently the most common and at the same time the least studied lesions of the gastrointestinal tract. The mechanism of development of erosions, which are small (up to 3-4 mm) foci of necrosis of the mucous membrane in depth to a certain level (up to the so-called muscular lamina propria) and heal without scar formation, unlike ulcers, has not been fully elucidated.
Currently, depending on the structure, quantity and homogeneity, acute (the defect heals within 4-9 days) and chronic (healing over several months or years) erosions are distinguished.
According to the reasons for the development of gastric erosion, they are divided into:
- Primary, developing without concomitant diseases;
- secondary, which arise as a systemic lesion during severe injuries, burn disease, and stress.
Causes of gastric erosion
Currently, erosive gastritis of the stomach does not have a unified theory of occurrence. There are risk factors that increase the likelihood of developing erosive gastritis:
- Firstly, Helicobacter pylori infection. There is no direct evidence that this bacterium causes erosion. However, its eradication (removal) from the gastric mucosa sharply shortens the treatment time and increases the recovery rate of patients suffering from erosive gastritis.
- Secondly, the developing reflux of bile and bile acids with insufficiency of the sphincter between the stomach and duodenum, disruption of the movement of the food bolus into the underlying sections of the gastrointestinal tract, in approximately a third of cases, become the causes of erosion.
- Thirdly, a state of constant stress and nervous tension, which lead to an increase in the level of adrenaline, cortisol, thyroxine, are the direct causes of the development of erosive gastritis against the background of complete well-being.
- Fourthly, long-term use of anti-inflammatory drugs (aspirin, paracetamol, diclofenac, etc.) can cause erosive damage to the gastric mucosa.
Symptoms of erosive gastritis
There are no specific symptoms for erosive gastritis. Acute erosion can be suspected by sudden onset of heartburn, sour belching, and abdominal pain on an empty stomach. However, in 90% of cases, acute erosions go unnoticed.
Chronic erosions disturb a person with more pronounced pain in the upper third of the abdomen and digestive disorders. Belching, heartburn, heaviness in the abdomen and increased gas formation over the course of several months become signs by which erosion can be suspected. You may also experience dull or cramping pain in the upper third of the abdomen on an empty stomach, which can radiate to the spine. Unstable stool appears with a predominance of constipation.
At the first suspicion of the development of acute or exacerbation of chronic gastritis, you should immediately consult a doctor to exclude the development of erosive gastritis.
Treatment of erosive gastritis
Choosing tactics for treating erosions of the stomach or duodenum is not an easy task. Since the mechanisms of erosive gastritis are not yet fully understood, treatment is aimed at all possible links in the development of the disease. A doctor treats erosive gastritis. Avoid self-medication.
The primary task is to remove Helicobacter pylori from the gastric mucosa, for which three- and four-component regimens are used (see “Treatment of gastritis”).
Erosive gastritis: treatment with folk remedies
Treatment using traditional medicine recipes has no independent meaning. It is effective only in complex therapy with medications (see “Treatment of gastritis”).
Superficial gastritis
This form of gastritis was established solely thanks to the introduction of a special diagnostic method - fibroesophagogastroduodenoscopy (FEGDS). This diagnosis is made solely by microscopic examination of pieces of the gastric mucosa under a microscope. The characteristic changes that are detected in this case predominate with inactive gastritis or gastritis in the stage of long-term remission.
Its isolation became necessary due to the fact that this form of inflammation of the gastric mucosa is the first sign of the disease transitioning to the chronic stage and the eligibility for the diagnosis of “chronic gastritis”.
It is believed that with this type of inflammation of the gastric mucosa there are no significant disturbances in the structure of the cells, their functions are mostly preserved. However, increased secretion of mucus is already observed, and the production of hydrochloric acid and pepsinogen, the main enzyme of gastric juice, is slightly reduced. These changes are not yet pronounced and total, as with atrophic gastritis, but can further progress.
Symptoms of superficial gastritis
For this type of gastritis, typical symptoms (pain, discomfort in the upper third of the abdomen after eating or on an empty stomach, disruption of digestion and metabolism) are not typical. Superficial gastritis in the vast majority of cases is asymptomatic or only with minor manifestations. Most often, superficial gastritis becomes a finding during routine systematic examinations that are carried out in risk groups. They are workers in hazardous industries (heavy industry, chemical production, people with a family history of autoimmune diseases, etc.)
Treatment of superficial gastritis
If this type of gastritis is detected, no specific treatment is required. General strengthening therapy is prescribed, planned treatment of chronic foci of infection (carious teeth, chronic sinusitis, pustular skin lesions, etc.) is carried out, and the intake of multivitamin complexes and minerals is recommended. It is necessary to give up bad habits (smoking, drinking alcohol), moderate gastronomic excesses (overeating, excess spices, salt, smoked meats, marinades, carbonated water) in the daily menu. In general, the diet for superficial gastritis is looser than for other types of inflammation of the gastric mucosa (for more detail, see “Treatment of Gastritis”).
Drug treatment consists of a course of medications that stimulate the restoration of stomach cells and the treatment of concomitant diseases.
It should be remembered that at this stage of the development of the disease, the process of changes in the gastric mucosa is manageable - disciplined implementation of the doctor’s recommendations can protect against the transition of this type of gastritis to subsequent forms with the ensuing consequences.
γαστήρ (gaster) “stomach” - inflammatory or inflammatory-dystrophic changes in the mucous membrane) is a long-term disease, characterized by dystrophic-inflammatory changes in the gastric mucosa, occurs with impaired regeneration, also with atrophy of epithelial cells and replacement of normal glands with fibrous tissue. The progression of the disease leads to disruption of the basic functions of the stomach, primarily secretory.Gastritis is a morphological diagnosis that may have no clinical equivalent and be asymptomatic. And the clinical diagnosis, the complaints presented by the patient, fit into the diagnosis of functional dyspepsia, with the leading variant for it (epigastric pain syndrome, or post-prandial distress syndrome).
So, by unreasonably diagnosing chronic gastritis (without confirming it with a morphological examination of the biopsy), the doctor takes upon himself responsibility, since this is a potentially precancerous disease and such a group of patients should undergo medical examination. For degrees 1-2, - 1 time per year, with degree of atrophy 3-4, - once every 6 months.
Acute gastritis
Acute gastritis is an acute inflammation of the gastric mucosa caused by a single exposure to strong irritants. Acute gastritis often develops as a result of chemical irritants entering the stomach, taking certain medications, or eating low-quality food contaminated with pathogens. In addition, acute gastritis can also occur against the background of other general diseases, often with acute infections or metabolic disorders.
Depending on the clinical manifestations and the nature of damage to the gastric mucosa, the following types of acute gastritis are considered: catarrhal, fibrinous, corrosive And phlegmonous:
To eliminate pain, take antispasmodics, anticholinergics, and antacids. It is recommended to take enterosorbents (smecta and others). For vomiting, prokinetics are prescribed. For acute toxicoinfectious gastritis - antibiotics (aminoglycosides, fluoroquinolones, biseptol and others). In severe acute gastritis, glucose solution, saline solution, and potassium preparations are administered parenterally to correct water and electrolyte disturbances.
Chronic gastritis
Houston classification chronic gastritis:
- gastritis A - autoimmune characterized by the formation of antibodies in the parietal cells of the fundus due to the appearance of antigenic properties of the protein structures of the cells. This type of gastritis is accompanied by pernicious anemia (due to impaired production of Castle factor).
- gastritis B - bacterial ; due to infection Helicobacter pylori. This type occurs in 90% of cases of chronic gastritis.
- gastritis C - reflux -gastritis; due to the reflux of bile acids and lysolecithin into the stomach.
Other forms of gastritis also occur:
- granulomatous (in Crohn's disease)
Etiology of chronic gastritis
The appearance and development of chronic gastritis is determined by the influence of many factors on the stomach tissue. The main external (exogenous) etiological factors contributing to the occurrence of chronic gastritis are:
Internal (endogenous) factors contributing to the occurrence of chronic gastritis are:
Helicobacter pylori
Schematic representation of the pathogenesis of gastritis caused by Helicobacter: 1) Helicobacter pylori penetrates the mucus layer in the host's stomach and attaches to epithelial cells; 2) bacteria catalyze the conversion of urea into ammonia, neutralizing the acidic environment of the stomach; 3) reproduce, migrate and form an infectious center; 4) as a result of destruction of the mucous membrane, inflammation and death of epithelial cells, gastric ulcerations are formed
In the second half of the 20th century, a previously unknown factor was identified, which today is considered one of the first places in the etiology of chronic gastritis. Helicobacter pylori is a spiral-shaped gram-negative bacterium that infects various areas of the stomach and duodenum. Many cases of gastric and duodenal ulcers, gastritis, duodenitis, and possibly some cases of gastric lymphoma and gastric cancer are etiologically associated with infection Helicobacter pylori. Successful experience with self-infection of one of the pioneers of the role Helicobacter pylori in the development of diseases of the stomach and duodenum - Barry Marshall and a group of volunteers served as convincing evidence of this theory. In 2005, Barry Marshall and his colleague Robin Warren were awarded the Nobel Prize in Medicine for their discovery.
However, in the majority (up to 90%) of infected carriers Helicobacter pylori no symptoms of disease are detected. Not every chronic gastritis has a bacterial cause.
Classification
By etiology Chronic gastritis is divided into three main forms:
- type A(autoimmune) - fundic gastritis; inflammation is caused by antibodies to the lining cells of the stomach. Usually accompanied by the development of pernicious anemia;
- type B(bacterial) - antral gastritis associated with contamination of the gastric mucosa by bacteria Helicobacter pylori- accounts for up to 90% of all cases of chronic gastritis;
- type C(chemical) - develops as a result of the reflux of bile and lysolecithin into the stomach during duodenogastric reflux or as a result of taking certain classes of drugs (NSAIDs, etc.)
In addition, there are also mixed - AB, A.C. and additional ( drug, alcoholic, etc.) types of chronic gastritis.
Topographically distinguished:
- gastritis of the antrum of the stomach (pyloroduodenitis);
- gastritis of the fundus of the stomach (body of the stomach);
- pangastritis (common).
Chronic gastritis and functional dyspepsia
Chronic gastritis, manifested by persistent structural changes in the gastric mucosa, most often has no clinical manifestations. In Western countries, the diagnosis of “chronic gastritis” is rarely made recently; the doctor usually focuses on the symptoms of the disease and, on its basis, uses the term “functional dyspepsia”. In Russia, on the contrary, the diagnosis of “functional dyspepsia” is made very rarely; the diagnosis of “chronic gastritis” is used many times more often. In Japan, the country with the highest incidence of gastric cancer, the diagnoses of “chronic gastritis” and “functional dyspepsia” are combined, thereby indicating the presence or absence of changes in the gastric mucosa and/or corresponding clinical symptoms.
Clinical manifestations
Chronic gastritis is clinically manifested by both local and general disorders, which, as a rule, appear during periods of exacerbation:
- Local disorders characterized by symptoms of dyspepsia (heaviness and feeling of pressure, fullness in the epigastric region, appearing or intensifying during meals or shortly after meals, belching, regurgitation, nausea, unpleasant taste in the mouth, burning in the epigastrium, often heartburn, which indicates a violation of gastric evacuation and reflux of gastric contents into the esophagus). These manifestations more often occur in certain forms of chronic antral gastritis, which lead to impaired gastric emptying, increased intragastric pressure, increased gastroesophageal reflux and exacerbation of all of these symptoms. In chronic gastritis of the body of the stomach, manifestations are rare and are reduced mainly to heaviness in the epigastric region, which occurs during or shortly after eating.
- General disorders may be manifested by the following syndromes:
- weakness, irritability, disorders of the cardiovascular system - cardialgia, arrhythmia, arterial instability;
- patients with atrophic chronic gastritis may develop a symptom complex similar to dumping syndrome (sudden weakness, pallor, sweating, drowsiness, occurring soon after eating), sometimes combined with intestinal disorders, with an imperative urge to stool;
- in patients with chronic gastritis of the body of the stomach and the development of B12-deficiency anemia, weakness, increased fatigue, drowsiness appear, there is a decrease in vitality and loss of interest in life; there is pain and burning in the mouth, tongue, symmetrical paresthesia in the lower and upper extremities;
- in patients with Helicobacter pylori-associated antral chronic gastritis with high acidity, ulcer-like symptoms may develop, indicating a possible pre-ulcerative condition.
Diagnostics
Establishing a clinical diagnosis is based on determining the type of chronic gastritis, assessing the prevalence of morphological signs of the disease, the presence and severity of gastric dysfunction.
Stages of diagnosing chronic gastritis:
- Clinical diagnosis- the patient’s complaints, anamnesis, and examination data of the patient are analyzed, a presumptive diagnosis is made and a rational plan for instrumental examination is drawn up.
- Endoscopic diagnostics with mandatory biopsy - availability is determined Helicobacter pylori, the nature and localization of changes in the gastric mucosa, the presence of precancerous changes in the gastric mucosa. For a biopsy, at least 5 fragments are taken (2 from the antrum, 2 from the body of the stomach, 1 from the angle of the stomach).
- Respiratory diagnostics- availability is being confirmed Helicobacter pylori. This method involves the patient taking urea of normal isotopic composition and then measuring the ammonia concentration using a gas analyzer.
- Laboratory diagnostics- clinical blood test, biochemical blood test, clinical urine test, clinical stool test, stool occult blood test, detection of infection Helicobacter pylori.
- Ultrasound examination liver, pancreas, gall bladder - to identify concomitant diseases of the gastrointestinal tract.
- Intragastric pH-metry- determination of the state of secretion and diagnosis of functional disorders in acid-related gastrointestinal diseases.
- Electrogastroenterography- study of the motor-evacuation function of the gastrointestinal tract in order to determine duodenogastric reflux.
- Upper gastrointestinal manometry, with the help of which the presence or absence of reflux gastritis is determined (normally in the duodenum the pressure is 80-130 mm water column, in patients with reflux gastritis it is increased to 200-240 mm water column).
Relief of exacerbation of chronic gastritis
Treatment of relapse of chronic gastritis is carried out on an outpatient basis; the course of treatment, including diagnosis, is designed for 14 days. Among the medications for the treatment of chronic gastritis, proton pump inhibitors, H2-histamine receptor blockers, prokinetics, selective M-anticholinergics, and antacids are used. For some forms Helicobacter pylori- associated gastritis, eradication (destruction) is recommended Helicobacter pylori(see below)…
Eradication Helicobacter pylori
Among other forms of chronic gastritis, it predominates Helicobacter pylori- associated gastritis of the antrum of the stomach. For its treatment, the Maastricht III consensus meeting (2005) recommended a triple eradication regimen as first-line therapy, including one proton pump inhibitor and two antibacterial agents: clarithromycin and amoxicillin. If eradication fails, second-line therapy is proposed, including four drugs: a proton pump inhibitor, bismuth tripotassium dicitrate, metronidazole and tetracycline.
At the same time, a number of experts believe that, due to possible problems that may arise as a result of taking antibiotics, eradication should be carried out Helicobacter pylori makes no sense, although there is a chance that it will help. However, other doctors believe that some forms of gastritis, in particular Helicobacter pylori- associated atrophic gastritis, requires mandatory eradication Helicobacter pylori.
Reducing the acidity of gastric juice
In the treatment of chronic gastritis, antisecretory drugs and enveloping agents are actively used.
Medicines are used to suppress the secretion of hydrochloric acid in the stomach, which leads to a decrease in the acidity of gastric juice. The dose of antisecretory agents is selected individually.
Vitamin preparations are used as additional therapy: vitamin U (methylmethionine sulfonium chloride) and B5 (pantothenic acid). Vitamin U (methylmethionine sulfonium chloride) is involved in the methylation reactions of biogenic amines and thereby reduces gastric secretion and provides an analgesic effect. Pantothenic acid (vitamin B5) promotes healing of the mucous membranes of the gastrointestinal tract and stimulates intestinal motility. Excess hydrochloric acid in the stomach often occurs precisely when there is a lack of pantothenic acid in the body.
Diet
In case of exacerbation of gastritis, a gentle diet is necessary. Patients with gastritis are contraindicated in chocolate, coffee, carbonated drinks, alcohol, canned food, concentrates and substitutes of any products, herbs, spices, as well as fast food products, dishes that provoke fermentation (grapes, black bread, etc.), smoked, fatty and fried foods, pastry products. At the same time, food should be varied and rich in proteins and vitamins. After the end of the acute condition, nutrition should become complete, observing the stimulating principle during the period of remission in patients with low acidity. Small meals are recommended, 5-6 times a day.
Military medical examination
Examination of citizens with gastritis occurs in accordance with article 59 of the schedule of diseases. Depending on the degree of dysfunction, the conscript is assigned one of the following fitness categories.
Gastritis is a common pathology that affects the gastric mucosa. But not everyone knows that this term hides several subtypes of the disease - gastritis types A, B and C - each of which has different clinical manifestations and requires an individual therapeutic approach. Let's figure out what symptomatic picture each type of gastritis has, what modern methods of treatment and prevention are used.
Types of gastritis
The classification of types of gastritis of the stomach is carried out according to etiology, that is, based on the factor that provokes the development and progression of the disease.
Type A - autoimmune chronic gastritis
Type A gastritis is diagnosed in approximately 5% of cases, that is, its prevalence is low. The mechanism of damage to the gastric mucosa occurs as a result of disruption of the immune system.
The immune system produces cells that protect the body from foreign cells that are sources of potential danger. Antibodies attack antigens by destroying or binding them. But when the immune system malfunctions, antibodies attack not only foreign cells, but also the tissues of one’s own body.
Thus, autoimmune atrophic gastritis occurs due to an attack of antibodies on the cells of the gastric mucosa that produce enzymes and hydrochloric acid.
It is known that the hereditary factor is of no small importance in the occurrence of this pathology. Therefore, people whose relatives suffer from autoimmune gastritis should be extremely careful about measures to prevent diseases of the digestive tract.
Type B - chronic Helicobacter gastritis
Gastritis of this type is statistically much more common than other subtypes of the disease. The cause of its development is the bacterium Helicobacter pylori, which infects the tissues of the stomach and duodenum.
The toxins and urease produced by this bacterium contribute to damage to the lining of organs, and the bacteria themselves cause inflammation of these lesions. Trying to get rid of the source of inflammation, the stomach begins to produce even more hydrochloric acid, which corrodes the walls of the organ. Thus, gastritis develops first, and subsequently, without proper treatment, ulcers and stomach cancer.
- Helicobacter has a high degree of resistance to the environment. Most pathogenic bacteria die in the acidic environment of the stomach, but Helicobacter survives well in acid.
- You can become infected with it through dirty hands, saliva, or food.
- According to statistics, it can be found in the gastrointestinal tract of 70% of people.
Type C - chronic gastritis: reflux gastritis
This type of gastritis occurs as a result of reflux, in which the contents of the gallbladder enter the stomach, irritating its walls. A similar effect occurs with the abuse of alcohol and medications (mainly anti-inflammatory non-steroidal drugs).
It is important to know that sometimes a mixed type of gastritis occurs, in which the gastric mucosa is first attacked by Helicobacter bacteria, and then the immune system attacks the affected cells of the inflamed gastric mucosa.
Diagnostics

Diagnosis of gastritis of any type is key for quick and correct treatment. In its process, laboratory and functional diagnostic methods are used:
- clinical and biochemical blood tests that reveal the presence of an inflammatory process in the body (increased leukocytes and ESR) or confirm hyperchromic anemia as a marker of an autoimmune type of gastritis;
- stool analysis to detect traces of blood and undigested food, characteristic of all types of gastritis;
- fibrogastroscopy is a method of examining the stomach using a probe, which is inserted orally to study the condition of the mucous membrane on the device monitor;
- detection of Helicobacter using biopsy and microscopic examination of tissues;
- manometry is the main method used in the diagnosis of type C gastritis, which represents the pressure in the duodenum if it exceeds the norm of 130 mm Hg. Art., we can talk about the presence of reflux gastritis.
The symptomatic picture, that is, the patient’s complaints presented at an appointment with a therapist or gastroenterologist, is also important.
Gastritis type A
Autoimmune gastritis is rare, but its main danger is its incurability and hidden course. Therefore, it is useful for every person to know about the signs of the disease and nutritional rules that slow down the progression.
Symptoms
Autoimmune gastritis is asymptomatic for a long time, so the chance of diagnosing it at an early stage is almost minimal. The latent form of the disease can last for several years, after which anemia develops as a result of B12 deficiency. Therefore, the symptoms with which the patient comes to the doctor are more related to disruption of the nervous rather than the digestive system:
- weakness,
- fatigue,
- drowsiness.
When the disease becomes open, the patient experiences the following symptoms:
- dull pain in the abdomen, the occurrence of which does not correlate with the time of eating;
- nausea;
- unpleasant taste in the mouth;
- alternating constipation and diarrhea.

From the clinical picture it is obvious that this subtype of gastritis does not have specific symptoms associated with the functioning of the digestive system. Therefore, if this disease is suspected, the doctor first of all excludes gastritis types B and C, which are easier to diagnose using instrumental and laboratory diagnostics.
Treatment
There is currently no treatment for gastritis of autoimmune origin. Sometimes doctors use replacement therapy by prescribing enzymes to the patient. But the effectiveness of this treatment method has not been confirmed by clinical data.
For type A gastritis, it is important to treat magaloblastic anemia if it has been confirmed after bone marrow examination. For this purpose, the patient is prescribed lifelong intramuscular administration of the drug Oxycobalamin.
Diet principles
Diet for gastritis of autoimmune origin should be lifelong. Therefore, it is very important to adapt the doctor’s recommendations to your own taste preferences. In this case, it will be possible to slow down the progression of the pathology.
In order to simplify the cooking process, you should completely abandon frying in favor of using a steamer and oven.

Type B gastritis
Gastritis of bacterial origin is very common, but it is quite treatable with correct diagnosis, adequate treatment and a lifelong diet.
Symptoms
With gastritis caused by the Helicobacter bacteria, a person experiences the following symptoms:
- abdominal pain, mainly during hunger and at night;
- vomit;
- sour belching;
- constipation
The vast majority of symptoms are associated with increased stomach acid levels. This function of the body is protective: in this way the stomach tries to get rid of pathogenic bacteria that cause inflammation. But since Helicobacter pylori is resistant to hydrochloric acid, the acidity level of gastric juice constantly increases, causing a corresponding taste in the mouth and sour belching in a person.
Treatment
There are two approaches to the treatment of Helicobacter gastritis, which are called first-line and second-line therapy.
First-line therapy involves prescribing the following groups of drugs:
- antibiotics (Amoxicillin, Clarithromycin);
- antimicrobials (Metronidazole);
- proton pump blockers (Nolpaza, Controloc).
The duration of treatment is about 7 days.

Treatment with the second method requires the following prescriptions:
- antibiotics;
- antimicrobials;
- enveloping agents (Omeprazole, Omez);
- proton pump inhibitors (Lansoprazole, Pantoprazole);
- antihistamines (ranitidine).
The course of treatment lasts one week.
Only the attending physician can decide which therapeutic approach to use, based on:
- individual characteristics of the patient;
- his medical history;
- clinical picture.
Diet principles
The purpose of the diet is to minimize the mechanical traumatic effect of food on the gastric mucosa.
During the period of exacerbation of the disease, treatment in a hospital is necessary, where the patient is forced to follow a strict diet, which helps to quickly relieve the inflammatory process. But all doctor’s recommendations regarding nutrition must be strictly followed throughout life. Only in this case can remission be made lasting and the risk of complications of gastritis, which include stomach ulcers and cancer, reduced.
With bacterial gastritis, it is extremely important to avoid feelings of hunger. To prevent stomach pain and nausea from tormenting you at night, it is recommended to drink a glass of warm milk with honey before going to bed.
Gastritis type C
Gastritis, which occurs as a result of chemical damage to the mucous membrane, like the bacterial form, is very common. With the help of modern treatment and proper nutrition, you can quickly get rid of unpleasant symptoms and prevent exacerbation of the pathology.
Symptoms
Type C gastritis is often asymptomatic. As the disease progresses, a person may periodically experience:
- nausea,
- vomiting
- bloating,
- increased gas formation.
A specific sign of pathology is weight loss with a normal diet with sufficient calories.
Treatment

The goal of treating type C gastritis is to normalize intestinal motility and neutralize bile acid in the stomach. For this purpose, the following drugs are used:
- Motilium;
- Maalox;
- Phosphalugel.
It is important to note that self-medication is inadmissible, since gastritis can be caused by obstruction of the duodenum. Drug treatment does not bring any effect, and the disease itself can develop into oncology. In this case, surgical treatment is used.
Diet principles
A diet for this type of disease requires careful attention not only to the work of the stomach, but also to the activity of the intestines.
For all three types of gastritis, you need to follow fractional meals, in which food is taken in small portions every 3 hours. You should completely avoid eating on the go, and in case of an emergency, have a snack with you from the list of allowed foods.
Prevention
Preventing the development of gastritis is a completely feasible task for any person. Even the risk of the autoimmune form can be significantly reduced if disruptions in the functioning of the immune system are avoided: sources of chronic infection are promptly eliminated, and hypothermia and viral infections are avoided.
Prevention of gastritis includes the following recommendations:
- complete cessation of smoking;
- refusal or moderate consumption of alcoholic beverages with a good snack;
- fractional meals;
- refusal of canned food and fast food in favor of balanced healthy foods;
- avoiding stress;
- observing personal hygiene rules to avoid food poisoning.
You should regularly visit a doctor for preventive purposes in order to detect pathology at an early stage and get rid of it in time.